The prevalence of underlying health conditions that increase the risk of severe health outcomes related to COVID-19
Archived Content
Information identified as archived is provided for reference, research or recordkeeping purposes. It is not subject to the Government of Canada Web Standards and has not been altered or updated since it was archived. Please "contact us" to request a format other than those available.
Released: 2020-07-03
As the COVID-19 pandemic spreads, researchers and health professionals have noted large differences in the impact that the infection has on individuals. Whereas some remain asymptomatic and unaware of their infection or experience only mild symptoms, others require hospitalization, ventilation, and may even die. As research evidence accumulates, both nationally and internationally, it appears that certain health characteristics, such as obesity or the presence of chronic conditions, increase the risk of severe outcomes among those who are infected with the novel coronavirus.
To better understand which segments of the Canadian population may be vulnerable to severe health outcomes related to COVID-19, Statistics Canada and the Public Health Agency of Canada have worked collaboratively to build an index of underlying health conditions in the adult household population. Using information from the 2017/2018 Canadian Community Health Survey, new data tables released today estimate the proportion of the adult household population who may be at greater risk of severe health outcomes related to COVID-19 due to the presence of underlying health conditions.
Differences by age and sex
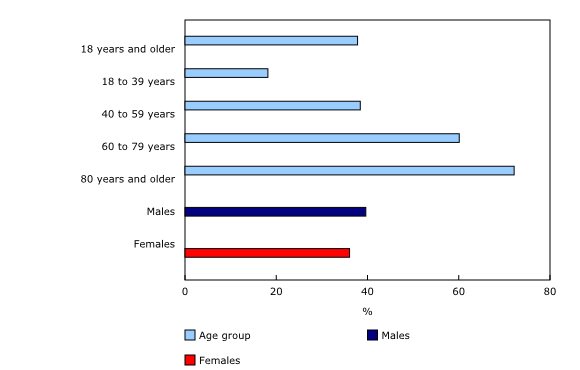
Overall, 37.8% of Canadian adults (age 18 and older) living in private households reported having one or more underlying health condition that could put them at elevated risk of complications following COVID-19 infection. In general, the proportion of individuals with underlying health conditions increased with age, and these conditions were more often reported among men (39.6%) than among women (36.1%).
Differences by region of residence
The newly released data also demonstrate that there are geographic differences in the proportion of adults reporting underlying health conditions. For example, 33.8% of adults in British Columbia reported having underlying health conditions, compared with 49.9% of adults in Newfoundland and Labrador. Some of this variability could be related to differences in the age structures and distribution of other factors (e.g., income levels) across provinces and territories. The data also provide estimates at the health region level, which show inter-provincial/territorial variations in underlying health conditions. Since health care is delivered at the health region level, these variations could help identify regions with greater needs.
Inequalities by income, Indigenous identity and cultural/racial background
In addition to geographic- and age-related differences, inequalities in health status across demographic and socio-economic characteristics continue to exist in Canada. The data released today show how the proportion of adult Canadians with underlying health conditions varies by educational attainment, household income level, Indigenous identity, and cultural/racial background.
The data shows an association between household income levels and the prevalence of underlying health conditions, whereby individuals living in higher income households are less likely to report having underlying health conditions than individuals living in lower income households. As shown in Chart 3, this relationship can be seen in most provinces across the country.
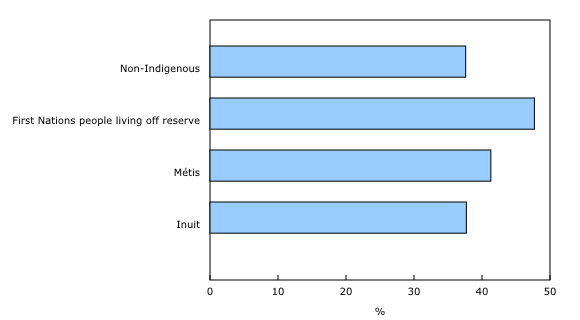
Individuals who self-identify as Indigenous are more likely to report underlying health conditions (44.4%) than those who identify as non-Indigenous (37.6%). Among the three Indigenous groups, those who identified as First Nations people (47.7%) had the highest prevalence of underlying health conditions, while those who identified as Métis (41.3%) or Inuit (37.7%) had lower prevalence.
Among non-Indigenous persons, 24.8% of those who identified as Arab/West Asian, 26.4% of those who identified as East/Southeast Asian, and 34.7% of those who identified as Black, reported having at least one underlying health condition, compared with 40.3% of those who identified as White.
The new data tables released today provide estimates of underlying health conditions by other socio-economic and demographic factors, nationally and at the level of province and territory.
Note to readers
The data released today were based on adult (age 18 years and older) respondents to the 2017/2018 Canadian Community Health Survey. Based on a review of the research literature regarding the health conditions that were most common among individuals who were hospitalized or who died due to COVID-19 infection, the following underlying health conditions were considered for respondents: chronic obstructive pulmonary disease (for respondents age 35 years and older), obesity (self-reported body mass index greater than or equal to 30), high blood pressure, currently having cancer, heart disease, suffering from the effect of a stroke, diabetes, or dementia (for respondents age 41 years and older). Individuals who reported that they had been diagnosed by a health professional with the considered health conditions, or whose self-reported height and weight classified them as obese, were assigned a score of 1 for each item. The number of conditions reported by each respondent was summed, for a possible total of 8. Individuals who were not asked about select health conditions due to their age (e.g., chronic obstructive pulmonary disease, dementia), or who otherwise did not respond to a particular item, were assigned a score of 0 for that item.
The data provide several breakdowns for the number of underlying health conditions reported by individuals: (i) one or more underlying health conditions, (ii) two or more underlying health conditions, (iii) three or more underlying health conditions, or (iv) four or more underlying health conditions. The assumption is that the presence of multiple underlying health conditions confers a greater level of risk than only one condition.
It should be noted that the data released today do not report specifically on individuals' infection status: the presence of underlying health conditions does not mean that an individual will become infected with the coronavirus. Rather, the data released today are meant to help identify groups of individuals who may be at greater risk of severe health outcomes if they were to become infected.
These data will also be made available in the Canadian Statistical Geospatial Explorer tool, which will allow users to visualize the differences in underlying health conditions across levels of geography.
Contact information
For more information, or to enquire about the concepts, methods or data quality of this release, contact us (toll-free 1-800-263-1136; 514-283-8300; STATCAN.infostats-infostats.STATCAN@canada.ca) or Media Relations (613-951-4636; STATCAN.mediahotline-ligneinfomedias.STATCAN@canada.ca).
- Date modified: