Publications
Aboriginal Peoples Survey, 2012
The Social Determinants of Higher Mental Distress among Inuit
The Social Determinants of Higher Mental Distress among Inuit
Archived Content
Information identified as archived is provided for reference, research or recordkeeping purposes. It is not subject to the Government of Canada Web Standards and has not been altered or updated since it was archived. Please "contact us" to request a format other than those available.
by Thomas Anderson

- Introduction
- Data source, concepts and methods
- Average mental distress score was higher for Inuit women than it was for men
- Higher mental distress population were more likely to have been diagnosed with a mood or anxiety disorder
- Suicidal thoughts were more likely for those in higher mental distress
- Inuit Tapiriit Kanatami's model
- Chronic conditions and food security were key predictors of mental distress for Inuit men
- Health care access and chronic conditions were strongly associated with mental distress among Inuit women
- Limitations
- Conclusions and next steps
- Appendix A
- Appendix B
- References
- Notes
Introduction
While mental health is an important issue to any population, it is of particular relevance to Inuit. Within the last decade, Inuit Tapiriit Kanatami—the national organization of Inuit in Canada—identified mental wellness as the single most important health issue for Inuit in Canada (Alianait Inuit-specific Mental Wellness Task Group, 2007).
Mental health is an indication of community and social well-being, affecting participation in all aspects of life (Herrman, Saxena, & Moodie, 2004). Negative mental health has been linked to a range of issues including a lack of social ties (Kawachi & Berkman, 2001; Kral et al., 2003), low-income (Caron & Liu, 2010) and chronic physical conditions (Scott et al., 2007). Furthermore, while mental distress is not the only relevant factor in suicidal thoughts or attempts, it has been shown to play a significant role (Ayalon, Mackin, Arean, Chen, & McDonel Herr, 2007).
Several short screening scales have been developed to monitor the prevalence of non-specific psychological distress, referred to in this paper as mental distress (Kessler et al., 2002). Mental distress is a strong, general indication of present-state mental disorders in a given population.
While analyzing mental distress among Inuit represents an important area of research, most studies that connect Inuit mental health to possible related factors tend to be qualitative in nature (Kirmayer et al., 2007; Kral et al., 2009; Tester & McNicoll, 2004). Furthermore, what quantitative studies do exist on Inuit health tend to be focussed on physical and general health outcomes as well as related factors (Bjerregaard, Young, Dewailly, & Ebbesson, 2004; Tait, 2008; Wallace, 2014) or are specific to suicide (Isaacs, Keogh, Menard, & Hockin, 1998).Note 1
Social determinants of health are defined as “the conditions in which people are born, grow, live, work and age, including the health system” (World Health Organization, 2014). Inuit Tapiriit Kanatami has developed its own set of social determinants that are applicable to Inuit health (Inuit Tapiriit Kanatami, 2014). This study uses Inuit Tapiriit Kanatami’s social determinants approach and data from the 2012 Aboriginal Peoples Survey to shed light on the types of circumstances, relationships and behaviours that are associated with mental distress among Inuit.
Start of text box
Data source, concepts and methods
2012 Aboriginal Peoples Survey
The 2012 Aboriginal Peoples Survey is a national survey of First Nations people living off reserve, Métis and Inuit aged 6 years and over as of February 1, 2012. It excludes people living on Indian reserves and settlements and in certain First Nations communities in the Yukon and the Northwest Territories. The survey was conducted from February 6 to July 31, 2012. Its sample of approximately 50,000 respondents was drawn from those who reported Aboriginal identity or ancestry on the 2011 National Household Survey (NHS).
The population of study was people who identified as Inuit on the 2012 APS. It was restricted to those aged 18 years and over, living in Inuit Nunangat.Note 2 Respondents who answered the survey by proxy were also excluded from this analysis, as they were not asked any of the questions on the K10 scale—this left a final sample of 2,571.
The Kessler distress scale
The ten-item Kessler Distress Scale (K10), as well as the shorter K6 version, have been validated in numerous studies and have been shown to reliably predict present-state mental health disordersNote 3(Kessler et al., 2002; Cornelius, Groothoff, van der Klink, & Brouwer, 2013). While no short-item scale could replicate a full, diagnostic psychological evaluation, the K10 derived variable provides a practical snapshot of the mental distress of a given population.
The 2012 APS used the K10 in order to enable the estimation of psychological distress. The scale was derived from ten questions on the 2012 APS. All questions contain the same introduction: “During the past month, that is, from [date one month ago] to yesterday, about how often did you feel”. The ten items are “tired out for no good reason”, “nervous”, “so nervous that nothing could calm you down”, “hopeless”, “restless or fidgety”, “so restless you could not sit still”, “sad or depressed”, “so depressed that nothing could cheer you up”, “that everything was an effort” and “worthless”.
Respondents were asked to rate the frequency of each item on a five-point scale (0-4), as occurring as little as “none of the time” to as often as “all of the time”. The results from each item were added together, giving each respondent a K10 score ranging from 0 to 40.
Prior to its inclusion on the 2012 APS, the K10 was never used on a national scale to assess the mental health of Inuit, though it was used for the total population in Canada (Caron & Liu, 2010). However, recent analysis assessed the psychometric properties of the K10 for the Inuit population, as well as Métis and First Nations people living off-reserve (Bougie, Arim, Kohen, & Findlay, forthcoming). The analysis demonstrated the unidimensional nature of the scale and its association with the other mental health concepts on the APS, such as the reporting of a mood or anxiety disorder, and the prevalence of suicidal ideation.
The analysis did not, however, suggest that the scale was a reliable diagnostic tool, since it was not validated against a comprehensive evaluation tool such as the Composite International Diagnostic Interview (CIDI). Without such a validation, it is impossible to assign definitive meaning to any particular score. Therefore the K10 has been treated simply as a measure of general mental distress, and not an indication of a mental disorder.
Methods of analysis
The outcome of interest in this study was higher mental distress as assessed by the K10 scale. A score on the K10 can range from as low as 0 to as high as 40. However, less than one percent of the sample population had a score of 30 or higher. When the sample was split into quintiles by K10 score, the upper quintile had a score of 9 or higher on the scale. This matches what was found for the total population in Canada in previous research (Caron & Liu, 2010). The upper quintile was used as a cut-off for identifying those with higher mental distress. A binary (yes/no) variable was generated with “yes” for those with a score of 9 or higher, and “no” for those with lower scores. This binary variable was used in analysis to identify potential social determinants of higher mental distress among Inuit.
Multivariate analysis was conducted using logistic regression, testing the probability of being in higher mental distress. Any differences noted in the paper are statistically significant, with a p-value of less than 0.05. The independent variables were chosen by using Inuit Tapiriit Kanatami’s conceptual model on the Social Determinants of Inuit Health as the guiding theory (Inuit Tapiriit Kanatami, 2014).Note 4
The mental health characteristics and the factors that are associated with mental health tend to differ for men and women (Langlois & Garner, 2013; Drapeau et al., 2010). Because of this, the logistic regression model was run separately for men and women; each calculated the probability of being in higher mental distress for selected characteristics. For both descriptive and multivariate analysis, variance was calculated using the bootstrap weights available on the APS master file.
Item non-response refers to responses of “don’t know”, “refusal”, and “not stated” to survey questions. Non-response counts were excluded from the calculation of descriptive statistics and for the dependent variable in the logistic regression model.Note 5 For all independent variables in the logistic regression model, non-response counts were included, but the data were not shown. For additional information on item non-response, please refer to the “Aboriginal Peoples Survey, 2012: Concepts and Methods Guide”
End of text box
Average mental distress score was higher for Inuit women than it was for men
In general, men and women have different physical and mental health characteristics and their health tends to be influenced by different factors. This has been noted specifically for the concept of mental distress (Langlois & Garner, 2013; Drapeau et al., 2010). Using the 2012 APS, the average mental distress score for Inuit women was higher than that of men (5.67 versus 4.77).
Higher mental distress population were more likely to have been diagnosed with a mood or anxiety disorder
Within the Inuit population, 5% reported having been diagnosed with a mood disorder, while 4% reported a diagnosis of an anxiety disorder.
As chart 1 illustrates, Inuit in higher mental distress were significantly more likely to have been diagnosed with a mood disorder than those who were not in higher mental distress (15% versus 2%E). The same relationship held true with anxiety disorders, as 11% of those in higher mental distress had been diagnosed with an anxiety disorder compared with 2%E of those who were not in higher mental distress.
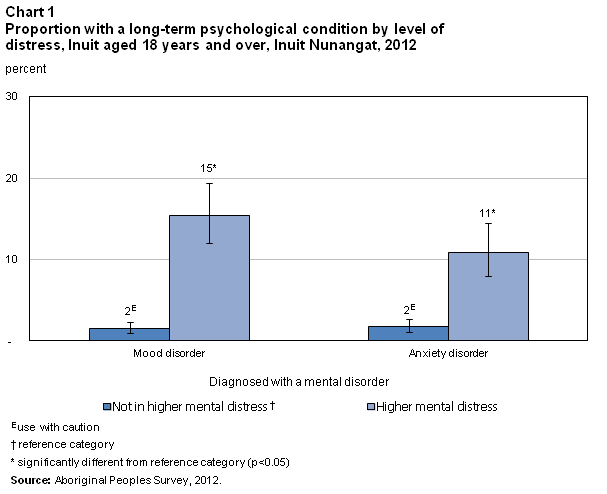
Suicidal thoughts were more likely for those in higher mental distress
Past research has demonstrated that Inuit suicide rates are between six and eleven times higher than the national average (Kral et al., 2003; Isaacs et al., 1998; Pike et al., 2010). On the 2012 APS, respondents were asked if they had ever seriously considered taking their own life.Note 6
In 2012, close to one-quarter (23%) of Inuit, aged 18 years and over, reported seriously considering taking their own life at some point in their lifetime. Of this group, more than one-quarter (26%) reported considering this in the past 12 months. Or, to put it differently, 6% of Inuit aged 18 years and over reported seriously considering taking their own life in the past 12 months. Inuit in higher mental distress were more likely to have considered taking their own life in the past 12 months than those who were not in higher mental distress (Chart 2).

Start of text box
Inuit Tapiriit Kanatami's model
To explore the social determinants of higher mental distress, associations were examined between higher mental distress and social determinants of Inuit health, which were adapted from Inuit Tapiriit Kanatami’s conceptual model on the Social Determinants of Inuit Health. This conceptual model was used as the theoretical framework for the logistic regression analysis (Figure 1). Nine of the eleven determinants put forward by Inuit Tapiriit Kanatami could be estimated using data from the 2012 APS.
Figure 1
Inuit Tapiriit Kanatami's model for the social determinants of Inuit health
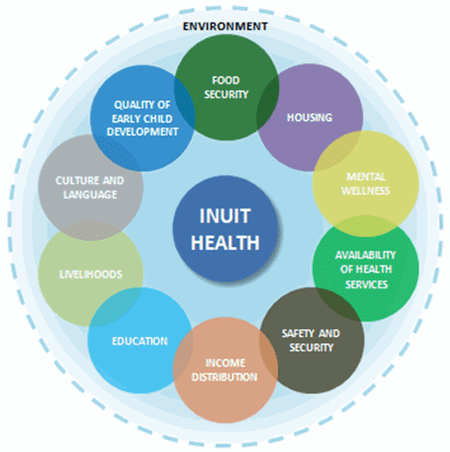
Source: Inuit Tapiriit Kanatami, 2014.
Variables from the 2012 APS were chosen to represent the social determinants in Inuit Tapiriit Kanatami’s model. The 2012 APS did not collect data that would allow for the study of the environment or the quality of early childhood development, meaning that these indicators could not be incorporated into the logistic regression. For more information on how the model was used and a list of definitions, see Appendix A.
End of text box
Chronic conditions and food security were key predictors of mental distress for Inuit men
Table 1 shows the unadjusted and adjusted probabilities of being in higher mental distress, for Inuit men aged 18 years and over. The unadjusted probability simply refers to the percentage that was in higher mental distress. The adjusted—or predicted—probability refers to the estimated likelihood of being in higher mental distress, when all other factors in the model are held constant.
When controlling for all variables, men who had been diagnosed with a chronic physical conditionNote 7 were more likely to be in higher distress than those who were not. Among Inuit men, the probability of being in higher mental distress was 30% for those with at least one chronic condition, compared with 15% of those who did not have any such condition. Food security was also associated with mental distress. The probability of being in higher mental distress was 26% for those with low or very low food security, compared with 10% for those with higher or moderate food security.
Inuit men who had been seriously injured in the previous 12 months were more likely to be in the higher mental distress group than those with no previous injuries (26% versus 18%), when controlling for all other factors. The adjusted probability of being in higher mental distress was also greater for those who reported an unmet health care need in the previous 12 months, compared with those who did not report an unmet need (27% versus 17%).
Respondents on the 2012 APS were asked to rate the strength of their family ties for those living in different households but in the same community. After adjusting for all other variables, Inuit men who reported strong or very strong family ties were less likely to be in higher mental distress (17%) compared with those who reported moderate to weak family ties (23%).
The legacy and impact of residential and federal industrial schools is well documented, extending into multiple generations (Spear, 2014). Inuit men who had attended a residential school or federal industrial school or who had a family member who attended were more likely to be in higher mental distress than those who did not (20% versus 12%), after adjusting for other variables.
Inuit men who had completed only high school were less likely to be in higher mental distress than those who had not completed high school (12% versus 21%). However, those who had completed only high school were also less likely to be in higher mental distress than those who had completed post-secondary education (12% versus 21%). This result, while counterintuitive, is consistent with existing literature on the mental health of Aboriginal people in Canada.Note 8
Health care access and chronic conditions were strongly associated with mental distress among Inuit women
The social determinants that were associated with higher mental distress for Inuit women were somewhat different than those for men. Table 2 shows the unadjusted and adjusted probabilities or being in higher mental distress for Inuit women.
When controlling for all other variables, the factors that were associated most strongly with mental distress among Inuit women were unmet health care needs and the presence of a chronic physical condition. If an Inuk woman had experienced a time in the previous 12 months when health care was needed but not received, her adjusted probability of being in higher mental distress was close to five-in-ten (47%); while the probability for those who did not report such an experience was just over two-in-ten (23%).
The adjusted probability of being in higher mental distress was 36% for Inuit women with a diagnosed chronic condition, compared with one-in-five (22%) of those who did not suffer from a chronic condition.
Lifetime drug use was also a related factor. Inuit women who had reported trying drugs at least once in their lifetime had a greater adjusted probability of being in higher mental distress (30%) than those who had never tried drugs (21%). It is important to note that the 2012 APS asked respondents if they had ever tried drugs but it did not ask about frequency of use or how recently drugs were taken.
Housing was correlated with mental distress for Inuit women—both household crowding and living in a dwelling in need of repairs. Three in ten (30%) Inuit women who lived in a crowded dwelling were predicted to be in higher mental distress, when adjusting for all variables, compared with 23% of those who did not live in a crowded dwelling. Among Inuit women who lived in a home that needed major repairs, 33% were predicted to be in higher mental distress, compared with 25% of those living in a home where only regular maintenance or minor repairs are needed.
Strength of family ties and food security were also associated with higher mental distress among Inuit women, when controlling for other factors. Inuit women who reported strong or very strong family ties were less likely to be in higher mental distress than those who reported moderate to very weak ties (24% versus 31%). Three-in-ten (30%) of those with low or very low food security were in higher mental distress, compared with more than two-in-ten (23%) of those with high or marginal food security.
Start of text box
Limitations
While care was taken to match appropriate variables to Inuit Tapiriit Kanatami’s model, every social determinant could not be included in the analysis. The lack of data on childhood development and the environment are significant limitations. Moreover, for those social determinants that could be measured, the variables used in the logistic regression model may only cover certain aspects of the determinants they represent.
Another limitation is that the 2012 Aboriginal Peoples Survey is a cross-sectional data source. As a result, it is not possible to determine any causal relationship between mental distress and the social determinants of health.
The K10 derived variable is a good general indication of mental distress. However, without analyzing the scale against a comprehensive diagnostic tool for the Inuit population, it lacks a defined cut-point. What can be said is that higher mental distress correlates strongly with other measures of mental illness, such as a diagnosed mood or anxiety disorder. Finally, although past analysis has demonstrated the scale’s strong psychometric properties for Inuit (Bougie et al., forthcoming), there may be unknown cultural biases that affect the interpretation of the questions on the K10.
End of text box
Conclusions and next steps
Mental distress is not the product of a single cause. Rather it is embedded within complex arrangements of circumstances, behaviours and relationships that are associated with mental health. Understanding these factors—often termed social determinants—may provide an opportunity to address negative mental health outcomes among Inuit.
While some similarities were found between the associated factors of mental distress for men and women, there were notable differences. Specifically, women who had ever tried drugs, lived in a crowded dwelling or in a dwelling in need of repairs were more likely to be in higher mental distress. These same variables did not, however, show a significant association to higher mental distress among Inuit men, after controlling for other variables. On the other hand, educational attainment (both less than high school and post-secondary completion), a personal or family history of residential school attendance and being injured in the past 12 months were significantly associated with higher mental distress for men.
For Inuit men and women, the presence of a physical chronic condition, low or very low food security, difficulties accessing health care and moderate to very weak family ties were all significantly related to higher mental distress, even after controlling for other variables.
There is a good deal more quantitative work that can be undertaken on the study of Inuit mental health. A longitudinal study of the correlates of mental distress among Inuit would be immensely valuable in determining some of the causes of poor mental health. Research on the prevalence of mental disorders within the Inuit population would also be of great use.
Special thanks
This paper would not have been possible without the support and guidance of Inuit Tapiriit Kanatami. In particular, I would like to thank Jesse Flowers and Tracy Sarazin for their involvement and care. Special thanks are also due to the study’s steering committee—Scott McLeish, Mohan Kumar and Leanne Findlay—who provided much needed expertise.
Appendix A
Inuit Tapiriit Kanatami’s conceptual model on the social determinants of Inuit health
The following represents the 11 social determinants of health from Inuit Tapiriit Kanatami’s model and— in cases where these determinants could be measured—how they were measured using APS data, in order to study their relation to mental distress.
1) Culture and Language
The last century brought dramatic change to Inuit culture and language. The ability to speak an Inuit language is cited as a “particular indicator of cultural well-being” (Inuit Tapiriit Kanatami, 2014). While family is “the foundation of Inuit culture” (Inuit Tapiriit Kanatami, 2015) and has been linked to Inuit mental health (Kral et al., 2003).
Language – This study categorizes the ability to speak an Inuit language using three levels: 1) speaks an Inuit language very well or relatively well, 2) speaks an Inuit language with effort or only a few words and 3) does not speak an Inuit language.
Strength of family ties– This variable refers to the reported strength of family ties—rated from 0 to 5—among family members living in a different household but in the same community. The relationship between strength of family ties was tested by positing “strong” or “very strong” reported ties (score of 4 or 5) versus responses of “moderate”, “weak”, “very weak” or “no family” (score of 3, 2, 1 or 0).
2) Livelihoods
Livelihood, within Inuit Tapiriit Kanatami’s framework is meant to “encompass a wide range of social factors beyond concepts such as employment” (Inuit Tapiriit Kanatami, 2014). In addition to a number of standard questions on participation in the labour force, the 2012 APS also asked respondents about a number of activities, outside of standard labour concepts, over the past year. These were:
- In the last year, did you make clothing or footwear?
- In the last year, did you make arts or crafts, for example, carvings, drawings, jewellery?
- In the last year, did you hunt, fish or trap?
- In the last year, did you gather wild plants, for example, berries, rice or sweet grass?
Employed or active in a traditional activity – If respondents were engaged in one or more “traditional activities” at least once per week or were employed at a job or business, they were considered “employed or active in a traditional activity”. If respondents were not employed or active in a traditional activity less than once per week, they were considered “neither employed nor active in a traditional activity”.
3) Income distribution
Income distribution is listed as a determinant of health, as the lack of income leads “to marginalization, limiting access to education, employment, good housing and nutritious food” (Inuit Tapiriit Kanatami, 2014).
Household income – This variable was defined as those below the median household income level versus those at or above the median household income level. The measure of income used was total household income, after-taxes and adjusted for household size.
4) Housing
Inuit Tapiriit Kanatami’s model defines adequate housing as “housing that is affordable (costing less than 30% of before-tax income), does not require major repairs and is not overcrowded” (Inuit Tapiriit Kanatami, 2014).
Dwelling in need of repairs – The 2012 APS asked respondents if their dwelling was in need of repairs. The variable was defined as a dwelling in need of minor repairs or regular maintenance only versus a dwelling in need of major repairs.Note 9
Household crowding – Calculating the number of persons per room is a common measure of household crowding.Note 10 This variable was defined as one person or fewer per room versus more than one person per room.
5) Personal safety and security
Inuit Tapiriit Kanatami’s model stresses the importance of safety and security to health. This encompasses a wide range of activities and characteristics, from high risk behaviours such as drug and alcohol abuse to the lasting impacts of residential schools. However, the survey did not ask respondents about issues such as violence or abuse.
Alcohol consumption – This variable was defined as those who had consumed alcohol in the last 12 months versus those who did not.
Drug use – This was defined as those who reported trying drugs in their lifetime versus those who reported no lifetime drug use.
History of residential school attendance – This was defined as the respondent having personal or family history of residential school attendance versus no family history of residential school attendance.
6) Education
Inuit Tapiriit Kanatami identified education as a key determinant of Inuit health. Education touches many aspects of life that are closely tied to health, such as income and livelihoods.
Highest level attained – This variable was defined as less than high school, versus those who completed high school and those who completed a post-secondary program. The category high school includes those who have taken some post-secondary education, but had not completed.
7) Food Security
Food security is defined as having “physical and economic access to sufficient, safe, and nutritious food to meet...dietary needs and food preferences for an active and healthy life” (Food and Agricultural Organization, 1996).
Level of food security – The food security scale on the 2012 APS was derived from six questions on the survey, which asked about personal and household food security. Two of the questions asked respondents about how often specific scenarios were true. These were:
- "The food that (you / you and other household members) bought just didn't last, and there wasn't any money to get more."
- "(You / You and other household members) couldn't afford to eat balanced meals."
The other four questions asked respondents if they skipped or cut the size of meals, the frequency of skipping or cutting meals, if the respondent ever ate less than they felt they should and if the respondent was ever hungry because they could not afford enough food. The variable was defined from this scale as those with high or marginal food security versus low or very low food security.
8) Availability of health services
The ability to access appropriate health care is of specific concern within Inuit Nunangat:
Access to health care is often limited in Inuit communities, many of which are served by a health centre staffed by a nurse or nurse practitioner. Moreover, recruitment, retention and training of health personnel are often issues that further hinder access to primary care.
(Wallace, 2014).
Difficulty accessing health care – The 2012 APS asked respondents if there was a time in the past 12 months when health care was needed but not received. The variable was then defined as those who answered “yes” versus those who answered “no”.
9a) Mental wellness
Within Inuit Tapiriit Kanatami’s model, mental wellness is considered a key determinant of Inuit health. While the APS has a number of mental health indicators beyond the distress scale, none of these should be viewed as social determinants of mental distress.
9b) Physical wellness
Alternatively, just as the model stresses the importance of mental wellness to overall health, this paper examines the inverse relationship between physical and mental health outcomes, which has been explored in numerous studies (Ormel et al., 1997; Scott et al., 2007).
Presence of a chronic condition – The APS asked respondents whether they had been diagnosed with a number of long-term conditions. The variable “presence of a chronic condition” was defined as having one or more chronic conditions that were diagnosed by a health professional versus no diagnosed chronic conditions. Within this paper, the presence of a chronic condition was limited to physical ailments only. Hence, respondents who reported a mood or anxiety disorder or a learning disability, with no other reported conditions, were not counted as persons with a chronic condition. The APS defines a “chronic condition” as a long-term condition that is expected to last or has already lasted at least 6 months, and that was diagnosed by a health professional.
Injuries – The 2012 APS asked respondents if they had been injured in the previous 12 months. The variable was defined as being injured in the past 12 months versus having no injury in the past 12 months.
10) Environment
The APS does not contain any variables that can capture either environmental factors by geography or environmental perceptions by respondents. As a result, this social determinant could not be analyzed.
11) Quality of Early Childhood Development
Childhood development cannot be properly captured using APS data. As a result, this concept could not be included in the logistic regression model.
Other variables
The multivariate analysis also controls for age and geography. However, the data for these variables were not shown in the analysis.
Age – Age was set as continuous with increments of 1 year.
Geography – The geography variable used was population centre size from the National Household Survey. It was defined as rural areas (less than 1,000 people) versus small population centres (1,000 to 29,999). There are no communities in Inuit Nunangat that are larger than 30,000.
Appendix B
| Variable | Description | percent |
|---|---|---|
| DDISTK10 | Derived variable - Distress scale - K10 | 12 |
| CC2_09 | Chronic health conditions - Mood disorder | 7 |
| CC2_10 | Chronic health conditions - Anxiety disorder | 7 |
| SU_01 | Suicide - Considered committing - Lifetime | 8 |
| SU_02 | Suicide - Considered committing - Past 12 months | 8 |
|
||
References
Alianait Inuit-specific Mental Wellness Task Group. (2007). Alianait Inuit Mental Wellness: Action Plan.
Ayalon, L., Mackin, S., Arean, P.A., Chen, H. & McDonel Herr, E.C. (2007). “The Role of Cognitive Functioning and Distress in Suicidal Ideation in Older Adults.” Journal of American Geriatric Society. 55(7), 1090-1094.
Bjerregaard, P., Young, T., Dewailly, E., & Ebbesson, S. (2004). “Indigenous health in the Arctic: an overview of the circumpolar Inuit population.” Scandinavian Journal of Public Health. 32(5), 390-395.
Bougie, E., Arim, R.G., Kohen, D. & Findlay, L.C. (in press). “Validation of the 10-item Kessler Psychological Distress Scale (K10) in the 2012 Aboriginal Peoples Survey.” Health Reports.
Caron, J. & Liu, A. (2010). “A descriptive study of the prevalence of psychological distress and mental disorders in the Canadian population: Comparison between low-income and non-low-income populations.” Chronic Diseases in Canada. 30(3), 84-94.
Cloutier, E. & Langlet, É., (2013). “Aboriginal Peoples Survey, 2012: Concepts and Methods Guide.” Statistics Canada Catalogue no. 89 653 X — no. 002.
Cornelius, BL, Groothoff, JW, van der Klink, JJ & Brouwer, S. (2013). “The performance of the K10 , K6 and GHQ-12 to screen for present state DSM-IV disorders among disability claimants.” BMC Public Health. 128(13).
Drapeau, A., Beaulieu-Prévost, D., Marchand, A., Boyer, R., Préville, M. & S. Kairouz. (2010). “A life-course and time perspective on the construct validity of psychological distress in women and men. Measurement invariance of the K6 across gender.” BMC Medical Research Methodology. 68(10).
Pike, I. et al. (2010). “Injury Prevention Indicators for Inuit Children and Youth.” Ottawa, ON: First Nations and Inuit Children and Youth Injury Indicators Working Group.
Food and Agricultural Organization of the United Nations. (1996). Rome Declaration on World Food Security. Accessed March 25, 2015.
Herrman, H., Saxena, S., & Moodie, R. (Eds.). (2004). Promoting Mental Health: Concepts, Emerging Evidence, Practice. Geneva: World Health Organization Press.
Inuit Tapiriit Kanatami. (2014). Social Determinants of Inuit Health in Canada. Ottawa: Inuit Tapiriit Kanatami. Accessed April 2, 2015.
Inuit Tapiriit Kanatami. (2015). Inuit Today. Accessed February 24, 2015.
Isaacs, S., Keogh, S., Menard, C. & Hockin, J. (1998). “Suicide in The Northwest Territories: A Descriptive Review.” Chronic Diseases in Canada. 198(4), 152-156.
Kawachi, I. & Berkman, L. (2001). “Social ties and mental health.” Journal of Urban Health: Bulletin of the New York Academy of Medicine. 78(3), 458-467.
Kessler, R.C., G. Andrews, L.J. Colpe, E. Hiripi, D.K. Mroczek, S.-L.T. Normand, ... Zaslavsky, A.M. (2002). “Short screening scales to monitor population prevalences and trends in non-specific psychological distress.” Psychological Medicine. 32, 959-976.
Kirmayer, L.J., Brass, G.M., Holton, T., Paul, K., Simpson, C., & Tait, C. (2007). “Suicide Among Aboriginal People in Canada.” Prepared for The Aboriginal Healing Foundation.
Kirmayer, L.J., Fletcher, C., & Watt , R. (2008). “Chapter 13: Locating the Ecocentric Self : Inuit Concepts of Mental Health and Illness.” In L.J. Kirmayer & G.G. Valaskakis (Eds.), Healing Traditions: The Mental Health of Aboriginal Peoples in Canada. (pp. 289-314). Vancouver: UBC Press.
Kral, M.J., Adams, E., Akoomalik, L., Allen, K., Arnaquq, E., Arnatsiaq, S., ... Wallace, D. (2003). “Unikkaartuit: Meanings of Well-Being, Sadness, Suicide, and Change in Two Inuit Communities.” Report submitted to National Health Research and Development Programs, Health Canada.
Kral, M.J., Wiebe, P.K., Nisbet, K., Dallas, C., Okalik, L., Enuaraq, N., & Cinotta, J. (2009). “Canadian Inuit Community Engagement in Suicide Prevention.” International Journal of Circumpolar Health. 68(3), 292-308.
Kumar, M.B. (forthcoming). “Lifetime suicidal thoughts among adult First Nations living off-reserve, Métis and Inuit adult (26-59 years) women and men: Prevalence and associated characteristics. ”Statistics Canada Catalogue no. 89-653-X.”
Langlois, K.A. & Garner, R. (2013). “Trajectories of psychological distress among Canadian adults who experienced parental addiction in childhood.” Health Reports. 24(3), 14-21.
Lucas, M., Dewailly, É., Blanchet, C., Gingras, S., & Holub, B.J. (2009). “Plasma omega-3 and psychological distress among Nunavik Inuit (Canada).” Psychiatry Research. 167, 266-278.
Lucas, M., Kirmayer, L.J., Déry, S. & Dewailly, É. (2010). “Erythrocyte N-3 Is Inversely Correlated with Serious Psychological Distress among the Inuit: Data from the Nunavik Health Survey.” Journal of the American College of Nutrition. 29(3), 211-221.
Ormel, J., Kempen, G.I., Penninx, B.W., Brilman, E.I., Beekman, A.T., & van Sonderen, E., (1997). “Chronic medical conditions and mental health in older people: disability and psychosocial resources mediate specific mental health effects.” Psychological Medicine. 27(5), 1065-1077.
Scott, K.M., Bruffaerts, R., Tsang, A., Ormel, J., Alonso, J., Angermeyer, M.C. . . . & Von Korff, M. (2007). “Depression–anxiety relationships with chronic physical conditions: Results from the World Mental Health surveys.” Journal of Affective Disorders. 103, 113-120.
Spear, W.K. (2014). Full Circle: The Aboriginal Healing Foundation & the Unfinished Work of Hope, Healing & Reconciliation. Ottawa: Aboriginal Healing Foundation.
Tait, H. (2008). “Aboriginal Peoples Survey, 2006: Inuit Health and Social Conditions.” Statistics Canada Catalogue no. 89-637-X2008001.
Tester, F.J. & McNicoll, P. (2004). “Isumagijaksaq: mindful of the state: social constructions of Inuit suicide.” Social Science & Medicine. 58(12), 2625-2636.
Wallace, S. (2014). “Inuit health: Selected findings from the 2012 Aboriginal Peoples Survey.” Statistics Canada Catalogue no. 89-653-X — no. 003.
World Health Organization. (2014). “Social Determinants of Health.” Accessed December 11, 2014.
Notes
- Date modified:
