Canadians with unmet home care needs
Archived Content
Information identified as archived is provided for reference, research or recordkeeping purposes. It is not subject to the Government of Canada Web Standards and has not been altered or updated since it was archived. Please "contact us" to request a format other than those available.

[Release from The Daily] [Full article in PDF]
- Overview of the study
- Introduction
- In 2012, 461,000 Canadians requiring help or care for a chronic health condition did not receive it
- Seniors less likely to have unmet needs
- Persons with lower incomes were more likely to have unmet needs
- Approximately 15% of care recipients considered that their needs were partially met
- Care recipients with a physical disability are more likely to have partially met needs
- Certain characteristics of the help received are associated with an increased probability of having partially met needs
- Several adverse effects for persons with unmet or partially met needs
- Conclusion
- Notes
- Related material for this article
Start of text box
Overview of the study
This article provides information on Canadians who require home care, but do not receive any (unmet needs), and on those who receive home care, but not enough (partially met needs). It also looks at the possible effects of a lack of help or care on a person’s well-being and mental health.
- In 2012, 2.2 million individuals, or 8% of Canadians 15 years of age and older, received help or care at home because of a long-term health condition, a disability, or problems related to aging.
- In 2012, nearly half a million Canadians, or 461,000 individuals 15 years and older, needed help or care in the 12 previous months for a chronic health condition, but did not receive it. They are referred to as persons with ‘unmet’ home care needs.
- Of the 2.2 million Canadians who received home care in 2012, 15% (331,000) did not receive all the help needed. They are referred to as persons with ‘partially met’ home care needs.
- Home care recipients with a physical disability were more likely to have partially met needs (18%) than care receivers without a disability (10%).
- Persons with unmet or partially met needs reported higher levels of stress and negative feelings. For example, 62% of care recipients with partially met needs experienced loneliness, compared with 31% of those whose needs were met.
End of text box
Introduction
Most seniors want to live at home as long as possible, even if they have a long-term health condition that limits their autonomy,Note 1 as do younger people with a chronic health condition or a physical or mental disability. Public authorities also also support the concepts of “home care” and “aging at home”, since they are generally less costly strategies.Note 2
To live at home safely and maintain an acceptable level of well-being, however, some people with a long-term health condition may require help with their daily activities (such as personal care, medical care, transportation, household maintenance or financial management). Do people who need help receive it? And if so, is the help received from family or paid professionals enough?
Finding the answers to these questions is important, because studies have shown that the risk of health deterioration, which may result in earlier institutionalization, increases significantly when home care needs are not met.Note 3 According to some studies, seniors who receive the most social support and professional home care services are less likely to be institutionalized.Note 4 Consequently, meeting the home care needs of individuals may encourage them to live in their homes over a longer period of time.
This article begins by discussing the number and proportion of persons living at home who reported that they needed care, but did not receive any (these will be referred to as persons with unmet need for home care). It then describes care recipients who received some help but not as much as needed (those with partially met needs). The last section shows, using various indicators, that persons with unmet or partially met needs were more at risk of experiencing stress, feelings of loneliness and a lower level of well-being.
Data for this article come from the 2012 General Social Survey (GSS) – Caregiving and Care Receiving. The GSS collects data on the situation of Canadians who receive help or care because of a long-term health condition, a disability, or problems related to aging. The target population for the GSS is all non-institutionalized persons 15 years of age and older living in the 10 provinces of Canada. Hence, the home care needs of institutionalized persons (for example, those in care facilities or retirement homes) are not covered in this study. A total of 23,093 respondents participated in the GSS (see box Data sources, methods and definitions).
In 2012, 461,000 Canadians requiring help or care for a chronic health condition did not receive it
In 2012, 2.2 million individuals, or 8% of Canadians 15 years and older, received help or care because of a long-term health condition, a physical or mental disability, or problems related to aging. They received help or care from family members, friends or professionals.Note 5
Seniors, especially older seniors, were by far the most likely to receive home care. In 2012, this was the case for 10% of those 65 to 74 years, 21% of those aged 75 to 84 and 45% of those 85 years and older.
These percentages may underestimate the number of persons needing help or care. In a recent report, the Health Council of Canada indicated that “there is no information in Canada to tell us how many seniors may be falling through the cracks – people who don’t have home care support, but probably should.”Note 6 Information on people who need help but don’t receive it was collected in the 2012 General Social Survey (GSS), not only for seniors, but also for younger people.
In 2012, nearly 461,000 Canadians 15 years of age and older reported that they had not received help, even though they needed it (during the 12 previous months for a chronic health condition). These persons represented 1.6% of the population 15 years of age and older. This proportion was slightly higher among those 75 and older, at just under 3% (Chart 1).
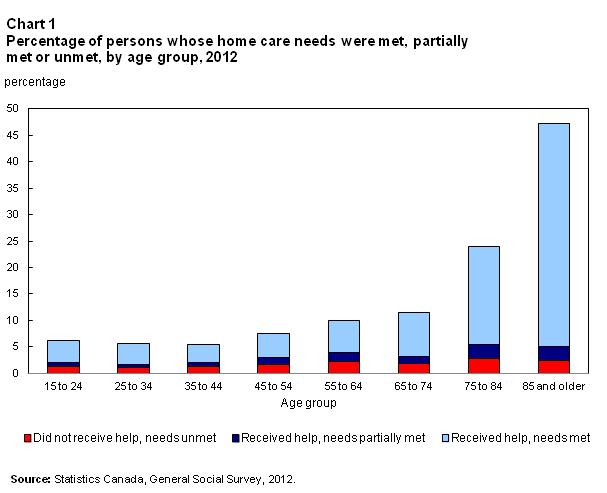
Of the 461,000 persons who needed help but did not receive it, slightly fewer than 290,000, or approximately two in three, had actually asked help, either from a family member or an organization. The other 170,000 consisted of those with no family members who could help or provide care, as well as those who did not want to request help for whatever reason. The proportion of those who had asked for help varied depending on age: it was 53% among individuals aged 65 and above, compared with 66% of those aged 15 to 64.
Seniors less likely to have unmet needs
Even though seniors were more likely than others to receive home care, they were proportionally less represented among those with unmet needs. Hence, 24% of individuals with unmet needs (nearly 110,000) were 65 and older, compared with 40% of those who were receiving home care.
This smaller representation was even more pronounced among the oldest seniors. While seniors 85 years and older represented 3% of those with unmet needs, they made up 12% of home care recipients (Table 1).Note 7 In terms of numbers, approximately 14,000 seniors 85 years and older living at home needed help or care but did not receive it, while 256,000 received home care.
| Persons who did not receive home care and did not need it | Persons with unmet needs for help or care | Home care recipients (ref.) | |
|---|---|---|---|
| thousands | |||
| Total | 25,996.3 | 461.1 | 2,162.0 |
| percentage | |||
| Total | 100 | 100 | 100 |
| Male | 50Note * | 42 | 43 |
| Female | 50Note * | 58 | 57 |
| Age group | |||
| 15 to 24 | 16Note * | 13 | 10 |
| 25 to 34 | 17Note * | 11 | 10 |
| 35 to 44 | 17Note * | 13 | 9 |
| 45 to 54 | 19Note * | 19 | 15 |
| 55 to 64 | 15 | 21Note * | 16 |
| 65 to 74 | 10Note * | 11 | 13 |
| 75 to 84 | 4Note * | 9Note * | 15 |
| 85 and older | 1Note * | 3Note * | 12 |
| Person living alone | |||
| No | 91Note * | 80 | 80 |
| Yes | 9Note * | 20 | 20 |
| Person has at least one type of physical disabilityTable 1 note 1 | |||
| No | 80Note * | 41Note * | 30 |
| Yes | 20Note * | 59Note * | 70 |
| Type of disabilityTable 1 note 2 | |||
| Communication-related (vision, hearing, speech) | |||
| No | 97Note * | 93Note * | 83 |
| Yes | 3Note * | 7Note E: Use with cautionNote * | 17 |
| Mobility problem | |||
| No | 98Note * | 83Note * | 63 |
| Yes | 2Note * | 17Note * | 37 |
| Pain and discomfort | |||
| No | 83Note * | 48 | 47 |
| Yes | 17Note * | 52 | 53 |
| Dexterity problem | |||
| No | 100 | 98 | 95 |
| Yes | 0 | 2Note E: Use with cautionNote * | 5 |
| Perceived health | |||
| Very good or excellent | 64Note * | 25 | 22 |
| Good | 29Note * | 34 | 33 |
| Fair or poor | 8Note * | 41 | 46 |
| Household income | |||
| Less than $20,000 | 4Note * | 18Note * | 12 |
| $20,000 to $59,999 | 22Note * | 30Note * | 32 |
| $60,000 or more | 49Note * | 29Note * | 33 |
| Not stated | 24 | 22 | 23 |
| Immigrant status | |||
| Canadian citizen by birth | 77Note * | 70Note * | 80 |
| Immigrant, refugee, non-permanent resident | 23Note * | 30Note * | 20 |
| Is a caregiver | |||
| No | 72 | 62Note * | 71 |
| Yes | 28 | 38Note * | 29 |
| Lives in a census metropolitan area or census agglomeration (CMA/CA) | |||
| Yes | 83Note * | 86Note * | 80 |
| No | 17Note * | 14Note * | 21 |
E use with caution
Source: Statistics Canada, General Social Survey, 2012.
|
|||
Baby boomers were actually the most represented among those who had unmet needs for home care. In 2012, 45- to 64-year-olds represented 40% of those who needed help or care but did not receive it, while they accounted for 31% of recipients.
Previous studies have also shown that seniors 65 and older were less likely to report that they had unmet needs for help or care.Note 8 There may be various reasons for this. First, seniors are more likely to have a regular doctor,Note 9 which may explain their greater propensity for reporting that they had received the help and care that they needed. Next, since a number of home care services are primarily intended for seniors, the health care needs of younger people, in particular 45- to-64-year-olds, may receive less attention. Finally, a certain number of seniors who may be the most likely to have unmet needs (e.g., those 85 and older) could be living in an institution (and are therefore not included in the survey).
The GSS collects data on various types of disabilities, both for those who receive home care and those who do not. Four types of physical disabilities are examined in this study: communication-related disabilities (vision, hearing and speech), mobility problems (ability to move), pain and discomfort, and dexterity problems (ability to move hands and fingers).Note 10
Not surprisingly, those with unmet needs for help or care were more likely to have at least one disability (59%) than those who did not receive care and did not need it (20%). However, home care recipients were the most likely to have a physical disability (70%). It should be recalled, however, that these care recipients are older than those with unmet needs.
This gap was reflected in the more specific types of physical disabilities. For example, 17% of persons with unmet needs had mobility problems, compared with 37% of those who received care at home.
In addition, among those with unmet needs for help or care, 7% had a communication-related disability (vision, hearing or speech), compared with 17% of individuals who received care at home. Persons with unmet needs were also less likely to have dexterity problems: 2% versus 5% of care recipients.
However, there was no significant difference for pain and discomfort as this condition was experienced by 52% of those with unmet needs and 53% of care recipients. There was also no difference in the degree of severity: the proportion of persons with pain and discomfort that limited most of their activities was the same for those with unmet needs and for care recipients (just under 20%).
Finally, those with unmet needs were as likely as home care recipients to perceive their health as being fair or poor (the difference was not statistically significant).Note 11
Persons with lower incomes were more likely to have unmet needs
Several studies have shown that persons with a lower socioeconomic status tend to be in poorer physical and mental health, are more likely to be sick and have a lower life expectancy.Note 12 For example, the life expectancy of 25-year-old males in the lowest income quintile is seven years shorter than that of males of the same age in the upper quintile.Note 13
GSS data, as well as results from other studies,Note 14 indicate that certain characteristics are associated with the probability of having unmet home care needs. Specifically, 18% of persons with unmet needs for help or care had a household income of less than $20,000, compared with 12% of those who received care at home and 4% of persons who did not need any care.
Similarly, immigrant status was associated with the likelihood of having unmet needs. Immigrants accounted for 30% of those with unmet needs for help or care and 20% of care recipients. Such a difference may partly be the result of immigrants’ social networks being less extensive and diverse than those of their Canadian-born counterparts.Note 15 Social networks matter because family and friends caregivers provide most of the hours of help given to care recipients.Note 16
Another group at higher risk of having unmet needs for help or care were the caregivers. Specifically, 38% of persons with unmet needs were providing help or care themselves, compared with 29% of care recipients and 28% of persons who did not need help.
Furthermore, a large portion of caregivers with unmet needs (35%) were providing 10 or more hours of care per week. These caregivers may be especially vulnerable, for they are also coping with the potentially stressful consequences of providing care to someone else, in addition to not receiving all the help they need.Note 17
Finally, persons who had unmet needs were less likely to live in regions located outside a census metropolitan area or census agglomerations (14%) than those who received home care (21%).
Approximately 15% of care recipients considered that their needs were partially met
Of the 2.2 million Canadians who received care in 2012 because of a long-term health condition, a disability or problems related to aging, some did receive care but not as much as they needed. They are referred to as persons with partially met needs. This part of the analysis looks at the characteristics of home care recipients who did not receive all the help they needed. It is important to identify characteristics associated with partially met needs, since persons with partially met needs are more likely to see their health deteriorate and require institutionalization.Note 18
In a previous Statistics Canada study, seniors were asked whether they had unmet professional home care needs for various activities.Note 19 The question in the 2012 GSS was more inclusive because care recipients were asked whether they had generally received all the help they needed in the previous 12 months, including help from professionals, friends and family members.
Of those who received home care in 2012, 85% felt that they had received all the help they needed during the year. The remaining 15%, or approximately 331,000 care recipients aged 15 years and older, reported that their needs for help or care were partially met (Table 2).
| Recipients who did not receive all the home care needed (needs partially met)Table 2 note 1 | ||
|---|---|---|
| in thousands | prevalence (%) | |
| Total | 330.9 | 15 |
| Male | 129.5 | 14 |
| Female | 201.4 | 17 |
| Age group | ||
| 15 to 24 | 31.6 | 14Table 2 note E: Use with caution |
| 25 to 34 | 29.5 | 13Table 2 note E: Use with cautionTable 2 note * |
| 35 to 44 | 36.1 | 18Table 2 note E: Use with caution |
| 45 to 54 | 66.8 | 21 |
| 55 to 64 (ref.) | 77.7 | 22 |
| 65 to 74 | 35.8 | 13Table 2 note * |
| 75 to 84 | 38.4 | 12Table 2 note * |
| 85 and older | 15.0 | 6Note E: Use with cautionTable 2 note * |
| Person living alone | ||
| No | 259.2 | 15 |
| Yes | 71.7 | 16 |
| Self-perceived health | ||
| Very good or excellent (ref.) | 34.1 | 7 |
| Good | 84.7 | 12Table 2 note * |
| Fair or poor | 209.0 | 22Table 2 note * |
| Person has at least one type of physical disability | ||
| No (ref.) | 59.3 | 10 |
| Yes | 266.2 | 18Table 2 note * |
| Type of disabilityTable 2 note 2 | ||
| Communication-related (vision, hearing, speech) | ||
| No (ref.) | 265.8 | 16 |
| Yes | 43.5 | 13 |
| Mobility problem | ||
| No (ref.) | 190.3 | 14 |
| Yes | 137.2 | 18 |
| Pain and discomfort | ||
| No (ref.) | 86.1 | 9 |
| Yes | 239.0 | 22Table 2 note * |
| Dexterity problem | ||
| No (ref.) | 310.0 | 15 |
| Yes | 18.8 | 17Note E: Use with caution |
| Main health condition for which the person received help or care | ||
| Arthritis or osteoporosis | 26.6 | 15Note E: Use with cautionNote du tableau 2* |
| Cardiovascular disease | 22.6 | 12Note E: Use with cautionNote du tableau 2* |
| Back problems (ref.) | 37.7 | 30 |
| Cancer | 17.4 | 11Note E: Use with cautionNote du tableau 2* |
| Mental health problem, or developmental disability or disorder | 56.3 | 14Note E: Use with cautionNote du tableau 2* |
| Other neurological diseases | 21.1 | 18Table 2 note E: Use with caution |
| Injury resulting from an accident | 39.0 | 18Table 2 note * |
| Old age | 13.7 | 7Note E: Use with cautionNote du tableau 2* |
| Household income | ||
| Less than $20,000 | 56.1 | 22Table 2 note * |
| $20,000 to $59,999 | 114.2 | 17 |
| $60,000 or more (ref.) | 95.6 | 13 |
| Immigration status | ||
| Canadian citizen by birth (ref.) | 258.0 | 15 |
| Immigrant, refugee, non-permanent resident | 66.5 | 16 |
| Is a caregiver | ||
| No (ref.) | 206.0 | 14 |
| Yes | 124.9 | 20Table 2 note * |
| Lives in a census metropolitan area or census agglomeration (CMA/CA) | ||
| Yes | 273.8 | 16 |
| No | 57.0 | 13 |
E use with caution
|
||
Seniors, who were less likely to have unmet needs, were also less likely, when receiving help, to perceive their needs as being partially met. Specifically, 6% of care recipients 85 and older and 12% of those aged 75 to 84 said that they had not received all the help they needed during the year. By comparison, the proportion was 22% among those aged 55 to 64. In addition to the reasons above (for example, more services for seniors, and some older, less healthy seniors living in institutions), different values and attitudes between generations may be behind these differences.Note 20
Care recipients with a physical disability are more likely to have partially met needs
Persons with unmet needs were less likely to have a physical disability (communication, mobility, pain, or dexterity problems) than those who received care. However, among care recipients with partially met needs, many had a disability.
In 2012, 18% of care recipients who had at least one physical disability reported not receiving all the help or care they needed, compared with 10% of care receivers who did not have a disability. Care recipients aged 15 to 64 who had a disability were even more likely to have partially met needs (approximately one in four, or 24%).
The higher prevalence of partially met needs among care receivers with a physical disability may be the result of these recipients needing more help than their family and friend caregivers or professionals were able to provide.Note 21 To illustrate, care recipients who had a physical disability received 25 hours of care per week on average, compared with approximately 13 hours for those who did not have a disability.
Of the various types of physical disabilities, pain and discomfort was the most strongly linked to the probability of having partially met needs (22% compared with 13% of those who had a communication-related disability). The proportion of care receivers with partially met needs was higher among those whose pain limited most of their activities, at 28% (representing approximately 115,000 individuals).
The main health condition for which a person receives home care was also linked to the likelihood of not receiving all the care needed. In particular, care recipients whose main health condition was a back problem were the most likely to report that not all their care needs were met (30%). By comparison, 12% of those receiving care because of heart disease reported not receiving all the help or care they needed. In terms of numbers, however, the largest group of persons with partially met needs were those who had a mental health condition (just over 56,000 individuals).
As previously shown, having a low income and being a caregiver were factors associated with the probability of having unmet needs. It appears that these factors were also related to the probability of having partially met needs.
Hence, 22% of care recipients whose household income was less than $20,000 reported not receiving all the help they needed, compared with 13% of those with a household income $60,000 or more. Low income individuals are more likely to have a disability and fair or poor health; they may also have less extensive social networks and fewer resources to pay for the help that they need.
As well, 20% of those who were caregivers felt that their own needs were not fully met, compared with 14% of non-caregivers.
Certain characteristics of the help received are associated with an increased probability of having partially met needs
In 2012, 45% of care recipients received help from both family members and professionals, 43% from family members only and 12% from professionals only. However, whether care was provided by family, friends or professionals did not affect the probability of having partially met needs (Table 3).
| Recipients who did not receive all the home care needed (needs partially met)Table 3 note 1 | ||
|---|---|---|
| in thousands | prevalence (%) | |
| Source of help | ||
| Informal caregivers and professionals | 143.6 | 15 |
| Informal caregivers only | 149.9 | 16 |
| Professionals only | 37.4 | 15 |
| Relationship with the informal caregiver (recipients 15 to 64 years of age) | ||
| Spouse | 101.6 | 22Table 3 note * |
| Children | 21.6 | 25Note E: Use with cautionNote du tableau 3* |
| Parents (ref.) | 45.4 | 13Table 3 note E: Use with caution |
| Other relative | 13.8 | 15Table 3 note E: Use with caution |
| Friends or neighbours | 28.6 | 28Table 3 note * |
| Relationship with the informal caregiver (recipients 65 and older) | ||
| Spouse | 28.4 | 11Table 3 note E: Use with caution |
| Son | 14.6 | 12Table 3 note E: Use with caution |
| Daughter (ref.) | 19.8 | 8Table 3 note E: Use with caution |
| Other relative | 3.6 | Table 3 note F: too unreliable to be published |
| Friends or neighbours | 8.1 | 17Note E: Use with cautionNote du tableau 3* |
| Number of hours of care received per week from professionals (all) | ||
| None | 172.5 | 16Table 3 note * |
| 1 hour | 54.2 | 16Table 3 note * |
| 2 to 9 hours | 78.6 | 17Table 3 note * |
| 10 hours or more (ref.) | 14.8 | 10Table 3 note E: Use with caution |
| Number of hours of care received per week from professionals (persons with a disability) | ||
| None | 140.0 | 20Table 3 note * |
| 1 hour | 37.4 | 19Table 3 note * |
| 2 to 9 hours | 67.2 | 19Table 3 note * |
| 10 hours or more (ref.) | 11.5 | 9Table 3 note E: Use with caution |
| E use with caution F too unreliable to be published
|
||
On the other hand, the specific relationship between care recipients and their primary caregivers could make a difference. Among 15- to 64-year-old care recipients, 28% of those who received help primarily from friends or neighbours and 25% of those who were helped by their children had partially met needs, compared with 13% of those who received care from their parents.
Among seniors 65 years and older, partially met needs were more prevalent among care recipients whose primarily caregivers were friends or neighbours (17%). By comparison, fewer seniors whose caregiver was the son (12%) or daughter (8%) felt that they had not received all the help they needed. Moreover, seniors without children—and therefore fewer potential family member caregivers—were more likely to have partially met needs (16% compared with 8% of seniors with four or more children).
Another factor that may be associated with an increased likelihood of having partially met needs is the number of hours of care received. However, among care recipients in 2012, there was no significant link between the total number of hours of care received and the likelihood of having partially met needs (between 15% and 16%). Similarly, the number of hours received from family and friends did not make a difference: the prevalence of partially met needs was the same for recipients who received one or two hours of care per week as for those who received 20 or more hours of care (16%).
In contrast, among those who received care from professionals, fewer hours of care were associated with higher levels of partially met needs. Specifically, approximately 17% of persons who received two to nine hours of professional care per week did not receive all the help they needed. By comparison, the proportion was 10% for those who received 10 or more hours of professional care per week.
The relationship between the number of hours of professional care and unmet needs was stronger among persons with a physical disability. Approximately 20% of care recipients who received nine or fewer hours of professional home care had partially met needs, compared with 9% of those who received 10 or more hours of professional care per week.
The factors associated with the probability of receiving all the help and care needed are often interrelated. For example, lower income can be associated with disability, poor health and less extensive support networks. However, when all the factors were considered simultaneously in a statistical model, the main findings remained basically the same: care recipients with a lower income and in poorer health were more likely not to receive all the help or care they needed. Recipients who received an average of 10 or more hours of professional home care per week were less likely not to receive all the care they needed. The total number of hours of care was not associated with the probability of having partially met needs.Note 22
Several adverse effects for persons with unmet or partially met needs
The difficulty some people have in getting help or care may be the result of various factors, such as insufficient social, family and financial resources, or a lack of government assistance. Regardless of the reasons, needing care and not receiving it may be associated with various consequences, such as stress, loneliness and sleep problems.
Studies have shown that feelings of loneliness could be associated with a decline in functional ability or even death.Note 23 The loneliness that some seniors may feel or that may arise after a loss of health or functional ability varied based on whether the person’s needs were met, unmet or partially met. Specifically, a feeling of loneliness was reported by 31% of those whose needs were met, 48% of persons whose needs were unmet and 62% of recipients whose needs were partially met (Table 4).
| Feeling of loneliness | High stress level | Sleep problems | |
|---|---|---|---|
| percentage | |||
| Home care or help status | |||
| Needs met (ref.) | 31 | 27 | 44 |
| Needs unmet | 48Table 4 note * | 35Table 4 note * | 58Table 4 note * |
| Needs partially met | 62Table 4 note * | 50Table 4 note * | 67Table 4 note * |
| predicted probabilitiesTable 4 note 1 | |||
| Home care or help status | |||
| Needs met (ref.) | 0.29 | 0.26 | 0.45 |
| Needs unmet | 0.47Table 4 note * | 0.32Table 4 note * | 0.58Table 4 note * |
| Needs partially met | 0.52Table 4 note * | 0.44Table 4 note * | 0.61Table 4 note * |
|
|||
As well, two-thirds of recipients (67%) with partially met needs reported sleep problems, compared with 44% of recipients whose needs were met. Persons with unmet or partially met needs were also more likely to describe most of their days as stressful.
A multivariate analysis taking into account other factors that can influence these negative perceptions (such as lower socioeconomic status or poorer health) substantiated the association between unmet or partially met needs and negative mental states. For example, accounting for other factors, the predicted probability of having sleep problems was 0.61 among recipients with partially met needs and 0.58 among those with unmet needs (a probability of 1 should be interpreted as a 100% chance of having partially met needs, while a probability of 0 indicate a 0% chance). By comparison, the probability was lower (0.45) among those who received all the help and care needed, the other factors remaining constant (needs met).
Conclusion
Given the aging population, meeting the needs of individuals with reduced autonomy or those who are limited in their daily activities is a challenge—especially when a person is facing a declining autonomy and has a lot of needs. In 2012, 2.2 million Canadians aged 15 and older received care from family and friends caregivers or professionals because of a long-term health condition.
Although most of those with needs for home care did receive help, some Canadians, namely 461,000 individuals 15 years and older, did not receive help in the previous 12 months even though they needed it. Those persons with ‘unmet’ needs were more represented in certain socioeconomic groups, specifically those with lower income, those 55 to 64 years of age and those who themselves were caregivers. Immigrants, who make up a growing share of the senior population, were also more likely to have unmet needs. Given the increasing diversity of future cohorts of immigrants, it will be interesting to see whether these trends continue into the future.
Of those who received care, some did not receive all the help they needed. These are referred to as persons with ‘partially met’ needs. In 2012, they totalled 331,000, or just over 15% of those who received care. As with unmet needs, the likelihood of being in such a situation varied depending on socioeconomic status and the type of care received. For example, recipients who received 10 or more hours of professional care per week were less likely to feel that their needs were partially met.Note 24
Lastly, this study has shown that persons with unmet or partially met needs for help or care were more likely to report negative emotional states. Even taking socioeconomic differences into account, persons with unmet or partially met needs reported a greater feeling of loneliness, more stress and sleep problems.
Martin Turcotte is a Senior Analyst in the Labour Statistics Division at Statistics Canada.
Notes
Additional information
Related Articles
Bibliographic references
- Date modified:
