Receiving care at home
Archived Content
Information identified as archived is provided for reference, research or recordkeeping purposes. It is not subject to the Government of Canada Web Standards and has not been altered or updated since it was archived. Please "contact us" to request a format other than those available.

by Maire Sinha and Amanda Bleakney
- Just over 2 million Canadians received care in 2012
- Most care receivers are women
- Mental illness was the single most common reason for care
- Men and women report similar conditions as reasons for care
- Four in ten care receivers report their health condition as severe
- Family and friends most common source of support
- Professional help more common for fibromyalgia, Alzheimer’s disease and mental illness
- Types of care from family and friends differ from professional services
- Care receivers typically receive help with many different types of activities
- Care recipients typically receive 7 hours of weekly care from family and friends
- Intensity of help highest for spousal care
- Care recipients with Alzheimer’s disease or dementia received the most hours of care
- Severity increases hours of family or friend care, but less so for professional care
- Most care receivers have been receiving help for over a year
- Emotional support not as common for those relying solely on professional care
- Most care receivers reported enough help, but not always from the source of their choice
- Summary
- Data source
- References
- Notes
In recent decades, there has been a growing shift away from institutional forms of care for Canadians with chronic health conditions or aging needs to an increased reliance on care within the home (Keefe, Hawkins and Fancy 2013). This emphasis on home care has accompanied changes in Canada’s age structure, with seniors representing a growing segment of the population, combined with the emergent preference for ‘aging in place’ - remaining at one’s home regardless of age or ability (Pynoos, Nishita, Cicero, and Caraviello 2008).
Receiving care at home is often considered a desirable option for Canadians requiring chronic, palliative or rehabilitative care. Many times, this is because they feel more at ease in familiar surroundings and are able to maintain some sense of independence (HHCA 2010). While the extent and nature of help needed and received can vary, so too can the source of care. Some care recipientsNote 1 receive help exclusively from family members, friends and neighbours, while others will combine this care with professional services. Finally, another segment may solely rely on professional help to meet their needs.
Using the 2012 General Social Survey (GSS), this report profiles care receiving in Canada, providing an understanding of Canadians who rely on care in the home.Note 2 Included in this discussion is an examination of the reasons for care, the types of people providing help, and the nature and intensity of care. The report concludes with a short discussion of satisfaction with the care received.
Just over 2 million Canadians received care in 2012
According to the 2012 GSS, 8% of Canadians aged 15 years and older received some form of care at home in the previous 12 months. This translates to 2.2 million Canadians relying on help to cope with a long-term health condition, disability or age-related needs.
These Canadians are a diverse group. They are not only seniors but also young and middle-aged adults. In 2012, just under one-third (29%) of care receivers were less than 45 years of age. Among this group were young under 25 years of age. They accounted for one in ten Canadians receiving some type of assistance in their own home (Chart 1). Another one in ten care receivers were between the ages of 25 and 34 years.
Nevertheless, as with previous findings, care receivers were still most commonly in their later years. One-quarter (27%) were in their mid-70s or older, with just less than half of this group aged 85 years or above.

Most care receivers are women
A slight majority (56%) of care receivers were women, partly reflecting their longer life expectancies and corresponding greater representation as seniors. Women accounted for 58% of all care receivers aged 65 to 74, and 65% of care receivers aged 75 and older.
Women’s higher representation as care receivers was not restricted to the senior years. Women represented the majority of care receivers for nearly all age groups, with the exception of the youngest. Between the ages of 15 and 34, men represented the slight majority of care receivers at 55%.
Mental illness was the single most common reason for care
The reasons underlying the need for care can vary.Note 3In 2012, mental health issues were the single most common, with one in seven Canadians (14%) reporting receiving care as a result of depression, schizophrenia, or other mental illness (Chart 2). Other common reasons for care included accident-related injuries (10%), aging needs (9%), cardio-vascular disease (9%), arthritis (8%), and cancer (8%).

Somewhat different reasons for care emerged for younger and older care receivers. Mental illness became much less common as people aged, with the reasons for care diversifying. For instance, while over one-third (35%) of care receivers under 25 years of age identified mental illness as the leading reason for care, this was the case for 12% of care receivers aged 55 to 64. This older group was equally as likely to say they were getting help to deal with cancer (13%).
Furthermore, mental illness was rarely mentioned as a reason for care among the senior population (2%E). Aging needs was the single most common reason for care among care receivers aged 65 years and older (23%).
Men and women report similar conditions as reasons for care
Men and women had similar reasons for receiving care. Notably, they were equally as likely to be receiving care for the two most common health conditions: mental illness and accident-related injuries.
A few gender differences were evident, yet these could be explained by age-related illnesses and gender-specific health conditions. Women were more likely than men to be receiving care for aging needs and arthritis, both related to the greater share of women as seniors. Other gender differences in reasons for care may be explained by differences in risk of health conditions. For instance, fibromyalgia, a condition typically affecting women, was almost exclusively a reason for care among women, while cardiovascular disease was a more common reason for care among men.
Four in ten care receivers report their health condition as severe
Canadians receiving care for a long-term health conditionNote 4 were asked about the severity of their condition. This could be related to their level of pain, prognosis, the chronic nature of the condition, and/or physical or mental capacity. Few care receivers reported a mild condition (18%) and most indicated that their condition was either moderate (38%) or severe (42%). The proportion reporting a severe condition was higher for certain health conditions, including fibromyalgia (67%), back problems (61%), arthritis (48%) and cancer (48%).
Family and friends most common source of support
Receiving care can come from a variety of sources. Most times, care receivers relied on the help of family and friends (88%), though half of these care receivers also received professional services. Relatively few Canadians (12%) relied on professional services alone.
For those relying on family and friends, nearly seven in 10 had more than one person helping them. Not unexpectedly, the closest family relationships were most often identified as the primary sources of care. In 2012, 39% of Canadians were primarily receiving help from a spouse or common-law partner, while 24% were receiving care primarily from a grown child and 19% from a parent (Chart 3). The least common caregivers were extended family members or siblings at 10%, and friends or neighbours at 8%.
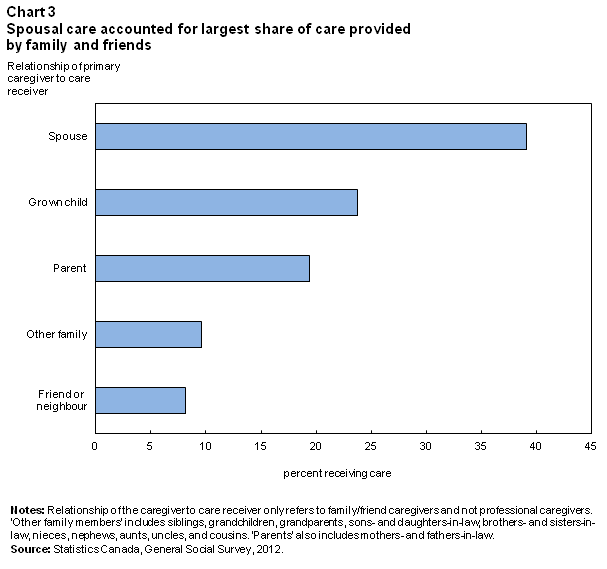
Overall, seven in ten care receivers lived in the same home as their primary caregiver. Virtually all spouses (98%) lived together, as did 78% of those primarily receiving care from a parent, 46% receiving care from a grown child and 33% receiving care from a friend.
Start of text box 1
Textbox 1: Trends in care receivingBox note 1
Across various sectors, the aging population has generated a growing interest and consideration into the needs and services for older Canadians. This has been particularly the case for the health care sector, including care of seniors within their own home. Using the GSS, it is possible to examine trends in family and friend-based care for Canadian seniors, as well as future seniors – those aged 45 to 64 years.Box note 2
In 2012, approximately 595,000 senior Canadians received care from family or friends for a long-term health condition in the previous 12 months. This represents about 12% of seniors, equal to the proportion of seniors receiving care in 2007. A similar stability in the prevalence of family or friend-based care was seen for younger Canadians. In both 2007 and 2012, 6% of Canadians aged 45 to 64 needed and received help from family and friends to cope with a long-term health condition.
Notes
End of text box 1
Professional help more common for fibromyalgia, Alzheimer’s disease and mental illness
The use of professional services, namely paid workers or organizations, may be influenced by an array of factors, such as need, availability of family and friend supports, cost and financial assistance. In general, professionals can be either licensed health professionals, such as nurses and physical therapists, or non-medical personnel whose role is to provide help with ‘activities of daily living’ (World Health Organization n.d.).
According to the 2012 GSS, professional services were generally more common for care receivers with certain health conditions. Care receivers with fibromyalgia, Alzheimer’s disease or dementia and mental illness were most likely to have used professional services in the previous year, while those with back problems were the least likely to have done so (Chart 4).
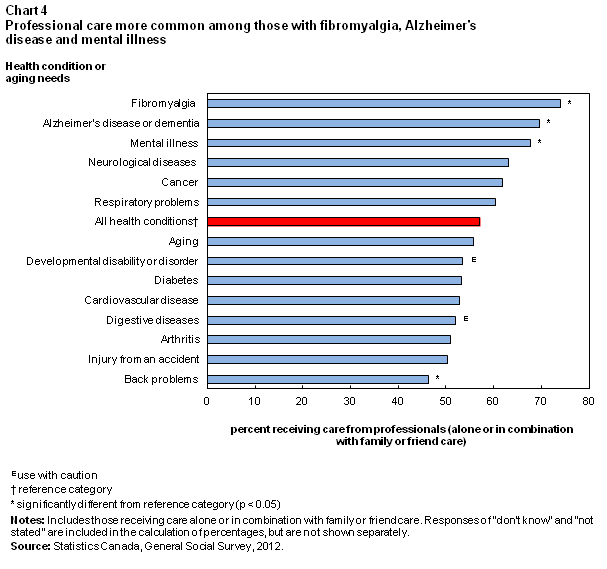
There was no difference in the use of professional services depending on the severity of the health condition. That is, care receivers with a severe or mild condition were equally as likely to receive professional help (61% versus 58%).
Start of text box 2
Textbox 2: Provincial variations in care receiving
The proportion of individuals receiving care for a long-term health condition, disability or aging needs was similar across Canada. The only exceptions were Newfoundland and Labrador, where the proportion was significantly higher (9%), and Alberta, where it was significantly lower (5%) (Textbox Chart). These differences were largely a reflection of varying levels of senior care, though for Alberta, levels of care were also lower for those under the age of 65.

As with the national picture, care receivers in all provinces typically relied on help from family and friends. However, care receivers’ use of professional services differed across Canada. Those in Newfoundland and Labrador were less likely to report using professional services, with less than half (46%) reporting this source of help in the last year. Conversely, at least two-thirds of care receivers in Quebec and Manitoba had received professional help.
End of text box 2
Types of care from family and friends differ from professional services
In addition to the source of care, care receivers were asked about the types of care they received. These responses were provided separately for family or friend-based care and professional services, due to the distinct differences in these two sources of support.
For family or friend-based care, receiving help with transportation topped the list of helping activities. Eight in ten care receivers (83%) had assistance with travel for running errands, attending medical appointments, or participating in social events. Help with indoor domestic tasks, as well as home maintenance or outdoor work were also very common, at 67% and 53%, respectively (Chart 5).
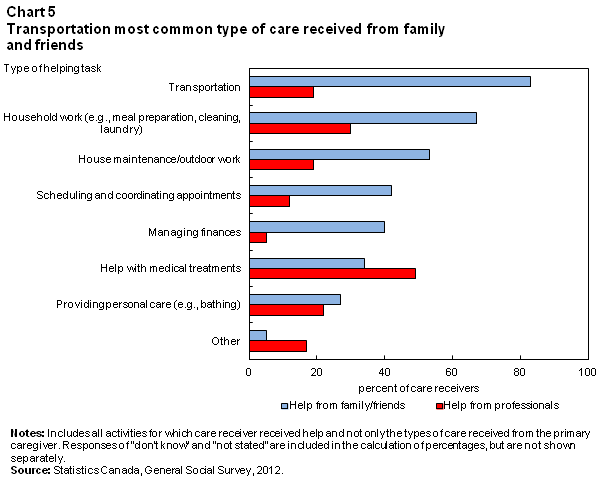
In comparison, the types of help received from professional services were more often medical in nature. Half (49%) of those receiving professional help had help changing bandages, measuring blood pressure, performing heart monitor tests, or other medical tests or treatments. Professional help for indoor domestic tasks, such as meal preparation and laundry, was a distant second at 30%, followed by receiving help with personal care, such as bathing, dressing or hair care (22%).
The home care services provided by professionals likely reflect their distinct roles and mandates, which may place limits on the types of help provided. For instance, help with transportation is often beyond the scope of their prescribed duties, and such activities may not be covered by employer insurance.
Care receivers typically receive help with many different types of activities
Receiving care often involved help with more than one type of activity. Typically, Canadians receiving help from family and friends had assistance with a median of three different activities, such as a combination of help with transportation, indoor domestic tasks, home maintenance and personal care. Seldom did family or friends help with a single task (16%). In fact, over half of care receivers (53%) reported having help with two to four tasks (Chart 6). Another 31% had help with five or more tasks.

Generally speaking, professional services provided help with fewer activities. Care receivers typically had help with a median of two activities from professionals. Indeed, help with a single activity was by far the most common for professional care, with half of care receivers (49%) reporting assistance in one area, such as medical or personal care. With each additional task, the share of professionals consistently decreased, meaning that very few care receivers (6%) were receiving professional help with five or more activities.
Care recipients typically receive 7 hours of weekly care from family and friends
Often closely tied to the number and range of tasks is the intensity of care, that is, the number of weekly hours of care. Overall, a median of 7 hours of care per week was reported by recipients of family or friend-based care. This weekly commitment of family and friends rose to 9 hours per week when care receivers had assistance with four types of tasks, and to 20 hours per week when care involved at least five or more different types of tasks.
Overall, professional care involved fewer hours of care than family or friend-based care. A median of 2 hours per week of professional care was reported by Canadians relying either partly or fully on professional services. No difference in the hours of professional care emerged whether the care recipient exclusively relied on professionals or supplemented this care with help from family and friends.
A number of factors may explain the difference in intensity of care provided by family and friends, and professionals. Care from family and friends typically involves a greater number of tasks, the caregiver may live in the same home, the caregiver may be more likely to have emotional bonds and/or perceived or actual obligations, and this care often involves multiple family and friend caregivers. In addition, the care receiver may not have financial resources for greater professional care.
Intensity of help highest for spousal care
For those receiving help from family and friends, variations in intensity existed based on the care receiver’s relationship with their primary caregiver. The hours of care were highest for spousal care. A median of 9 hours per week was reported by those receiving spousal care, 2 hours more than the median for family and friend care. Parents and children of caregivers reported the next greatest number of hours at 6E hours per week, followed by other family members, such as siblings and extended family (4E hours per week), and friends (4E hours per week).
Care recipients with Alzheimer’s disease or dementia received the most hours of care
The number of weekly hours of care was much higher for Alzheimer’s disease or dementia. Care recipients typically reported 37E hours a week of family or friend care. On the other hand, mental illness had below average weekly hours of family or friend-based care, at 3 hours. Part of the lower hours of care may be explained by need, as well as the supplementation with professional services. When care receivers did not have any help from professional services, the median hours of care from family and friends increased to 7E hours for those with mental illness.
Mental illness also had the lowest intensity of professional care, despite being a condition with a higher than average likelihood of professional care overall. There was no significant difference in the hours of professional services based on whether this care was combined with help from family or friends.
Severity increases hours of family or friend care, but less so for professional care
The severity of the health condition generally meant more hours of family or friend care. Overall, care receivers identifying a mild health condition reported about 4 hours of care per week, rising to 7 hours per week for a moderate condition, and 10 hours for a severe health condition. The severity of the health condition had a slight impact on hours of professional care. Those with a mild health condition received a median of one hourE of care per week, which rose to two hours of care for those with a severe health condition.
Most care receivers have been receiving help for over a year
While the intensity of care was measured in relation to the preceding 12 month-period, the vast majority (91%) had been receiving some form of help from family or friends for more than a year. In fact, about one in three care receivers (29%) had been receiving care from their primary caregiver for a decade or more. Receiving care for this period of time was more common among care receivers suffering from neurological diseases, such as Parkinson's disease (46%) and those dealing with age-related needs (39%).
Start of text box 3
Textbox 3: Engagement in the paid workforce
One in five care receivers too ill to work or engage in other main activity
Faced with a long-term illness, care receivers are sometimes unable to engage in their regular routines, whether it is paid work, child care, or some other main activity. Overall, 21% of care receivers indicated that they were too ill to work or to engage in other main activities over the last 12 months. These care receivers were most often between the ages of 45 and 64 and had a severe health condition. The intensity of family or friend-based care was also highest for these care receivers, as they received a median of 10 hours of care per week, higher than the median of 7 hours. There was no significant difference, however, in the level of professional services.
For some, having a long-term illness and receiving care did not preclude the possibility of participating in the paid workforce. In 2012, one in five care receivers identified their main activity as working at a paid job or business, rising to 32% when considering only those under the age of 65. Overall, these care receivers under the age of 65 had the lowest intensity of care. They reported a median of 5 hours of family or friend care, and 1 hour of professional care. They were also less likely to identify their condition as severe (30% versus 36%) and more likely to state that their condition was moderate (44% versus 33%).
Care receivers who did not work at a paid job or business were asked when they last worked. Among care receivers under 65 years of age who were not working at a paid job or business, about half (48%) indicated that they last worked in the previous five year period, while 31% said they had not worked in more than a decade. The proportion of care receivers working in the last five years was inversely related to the age, with the youngest being most likely to have worked in the past years and the oldest least likely.
Care receivers generally have lower incomes
The income of care receivers can be closely related to main activity, particularly when care receivers are unable to work due to their health condition. For those under 65 years of age, care receivers were twice as likely as other Canadians to have a household income of $40,000 or less (26% versus 13%). They were also less likely to report an income of $60,000 or more (40% versus 53%). The difference in household income between care receivers and other Canadians was most pronounced between the ages of 35 and 64.
Differences in household income were also apparent among seniors, but only for the lowest income levels. In 2012, 39% of senior care receivers had an income of $40,000 or less, compared to 31% of other seniors. Senior care receivers were equally as likely as other seniors to have a household income of $60,000 or more (22% and 24%).
End of text box 3
Emotional support not as common for those relying solely on professional care
Coping with a long-term illness or the challenges associated with advanced age can be emotionally difficult. Care receivers were asked whether they received emotional support. Overall, three-quarters (74%) indicated that a family or friend spent time with them, engaged in conversation, cheered them up or provided other forms of emotional support. Those receiving care from a combination of family, friends, and professionals were most likely to say that they were emotionally supported (80%), closely followed by those receiving care exclusively from family members and friends (75%).
For Canadians receiving help solely from professionals, emotional support was not as common. Over half (54%) said that they did not receive any emotional support from family and friends in the last 12 months. They were also unlikely to say that emotional help came from professionals, with just over one-quarter (28%) reporting that their professional caregivers were a source of emotional support.
Most care receivers reported enough help, but not always from the source of their choice
Regardless of the source of care, most care receivers (84%) felt that they received the care or help they needed in the past 12 months. At times, however, care receivers expressed a desire for another source of care. In 2012, 20% of those exclusively receiving care from family and friends would have rather had professional help and 15% of those exclusively receiving professional care would have rather had family or friend support.
Although the overall satisfaction with the balance of help from family, friends and professionals care was high (82%), care receivers who were dissatisfied stated that they would have preferred more professional help. In particular, 79% of dissatisfied care receivers said they needed more professional help. Another 18%E said they would have preferred more assistance from family and friends.
Start of text box 4
Textbox 4: Canadians not receiving care - Unmet needsBox note 1
The General Social Survey asked Canadians if they needed assistance to cope with a long-term illness, disability or aging needs, but did not receive any in the previous 12 months. In 2012, 2% of Canadians fell into this category, meaning that they had a long-term illness or aging needs but had to cope on their own. The majority (63%) of these people indicated that they had asked family and friends for some support, but did not receive any.
Among those who did not request any help, 39% said that they could have received some type of help if they had asked. Another 33% felt that help was unlikely and 28% were unsure.
Canadians without a long-term illness or age-related conditions were generally positive about the possibility of help, if needed. About 8 in 10 Canadians felt that they would get support from family and friends if help was required.
Notes
End of text box 4
Summary
Receiving care at home was a reality for 2.2 million Canadians or 8% of the Canadian population aged 15 years and over. Senior care receivers represented the largest segment of care receivers. Unlike their younger counterparts who were most often coping with mental illness, senior care recipients often received help to deal with age-related needs. Overall, mental illness was the most commonly reported reason for care, followed by accident-related injuries, age-related needs and cardiovascular disease.
In most cases, care receivers relied on the help of family and friends, though they often combined this care with help from professionals. Few Canadians relied on professional services alone. In general, care from family members or friends tended to differ from help from professionals, involving a greater range and number of tasks, and differing in nature and intensity.
Most felt that they received the care or help they needed in the past 12 months and did not prefer other sources of care. However, a need for greater professional services was mentioned for those who were dissatisfied with the balance of help from family, friends and professionals.
Data source
This article is based on Cycle 26 of the General Social Survey (GSS) on “Caregiving and Care receiving”. The objectives of this survey are to provide estimates of caregiving and care receiving in Canada and the characteristics of care receivers and caregivers.
Sampling
The target population included all persons 15 years and older living in the ten provinces of Canada, excluding full-time residents of institutions. In 2012, all respondents were interviewed by telephone. Households without telephones or with only cellular phone service were excluded. Based on the most recent Residential Telephone Services Survey, conducted in 2010, these two groups combined represented approximately 14% of the target population. This proportion may be higher for 2012 due to the likely increase in cellular-only households. Survey estimates were adjusted (weighted) to represent all persons in the target population, including those without telephones. Once a household was contacted, an individual 15 years or older was randomly selected to respond to the survey. The sample size in 2012 was 23,093 respondents.
Data collection
Data collection took place from March 2012 to January 2013 inclusively. Computer assisted telephone interviewing (CATI) was used to collect data. Respondents were interviewed in the official language of their choice. Proxy interviews were permitted. These represented 4% of all interviews.
Response rates
The overall response rate was 65.7%. Types of non-response included respondents who refused to participate, could not be reached, or could not speak English or French. Survey estimates were weighted to represent the non-institutionalized Canadian population aged 15 years or over.
Data limitations
As with any household survey, there are some data limitations. The results are based on a sample and are therefore subject to sampling error. Somewhat different results might have been obtained if the entire population had been surveyed. This article uses the coefficient of variation (CV) as a measure of the sampling error. Any estimate that has a high CV (over 33.3%) has not been published because the estimate is too unreliable. In these cases, the symbol ‘F’ is used in place of an estimate in the figures and data tables. An estimate that has a CV between 16.6 and 33.3 should be used with caution and the symbol ‘E’ is referenced with the estimate. Where descriptive statistics and cross-tabular analysis were used, statistically significant differences were determined based on a p value of 5%.
References
Chappell, Neena L., and Laura M. Funk. 2011. "Social Support, Caregiving, and Aging." Canadian Journal on Aging. 30.3: 355-370.
Cranswick, Kelly. 2002. General Social Survey Cycle 16: Caring for an aging society. Statistics Canada. Catalogue no. 89-582-XIE.
Denton, Frank T., and Byron G. Spencer. 2010. "Chronic Health Conditions: Changing Prevalence in an Aging Population and Some Implications for the Delivery of Health Care Services." Canadian Journal on Aging. 29.1: 11-21.
Evans, R.G., McGrail, K.M., Morgan, S.G., Barer, M.L. & Hertzman, C. 2001.”Apocalypse no: Population aging and the future of health care systems.” Canadian Journal on Aging, 20(1), 160-191.
Home Health Care Agencies (HHCA).2010. Benefits of Home Health Care. (accessed January 21, 2014).
Keefe, Janice, Glenda Hawkins, and Pamela Fancey. 2013. A portrait of unpaid care in Nova Scotia. Healthy Balance Research Program. 1-62.
Laurent, Martel. 2013 (September). “Mortality: Overview, 2010 and 2011.” Report on the demographic situation in Canada. Statistics Canada. Catalogue no. 91-209-X.
Pynoos, Jon, Christy Nishita, Caroline Cicero, and Rachel Caraviello. 2008. "Aging in place, housing, and the law." Elder Law Journal. 16.1: 77-105.
Scott, K.M., M. Von Korff, J. Alonso, M. Angermeyer, E.J. Bromet, R. Bruffaerts, G. de Girolamo, R. de Graaf, et al. 2008."Age patterns in the prevalence of DSM-IV depressive/anxiety disorders with and without physical co-morbidity." Psychological Medicine. 38.11: 1659-1669.
Stewart, M.J., A. Neufeld, M.J. Harrison, D. Spitzer, K. Hughes, and E. Makwarimba. 2006."Immigrant women family caregivers in Canada: implications for policies and programmes in health and social sectors ." Health & Social Care in the Community. 14.4 : 329-340.
Wilson, Coralie J., Debra J. Rickwood, John A. Bushnell, Peter Caputi, and Susan J. Thomas. 2011. "The effects of need for autonomy and preference for seeking help from informal sources on emerging adults' intentions to access mental health services for common mental disorders and suicidal thoughts." Advances in Mental Health. 10.1: 29-38.
World Health Organization (WHO). n.d. "Classifying health workers: Mapping occupations to the international standard classification." Classification of health workforce statistics. (accessed March 26, 2014).
Notes
- Date modified:
