Violent victimization of Canadians with mental health-related disabilities, 2014
Archived Content
Information identified as archived is provided for reference, research or recordkeeping purposes. It is not subject to the Government of Canada Web Standards and has not been altered or updated since it was archived. Please "contact us" to request a format other than those available.
by Marta Burczycka
Highlights
- An estimated 1 million Canadians live with a mental health-related disability, including anxiety, depression, bipolar disorder, anorexia, substance abuse and other conditions which limit their daily lives. According to the 2014 General Social Survey (GSS) on Canadians' Safety (Victimization), one in ten people with this kind of disability experienced violence in the preceding 12 months. This was more than double the proportion than among Canadians in general.
- Women with a disability related to mental health were more likely to experience violent victimization than their male counterparts (11% versus 8%). Sexual assault was especially prevalent among these women: 7% reported that they had experienced a sexual assault in the previous year, compared to 2% of women with no mental health disability.
- While research suggests that the relationship between violent victimization and mental illness is bidirectional—that is, mental illness may develop following victimization, or may increase vulnerability to victimization in the first place—developing symptoms consistent with Post-Traumatic Stress Disorder following victimization was more common among those with a mental health-related disability (29% versus 11%). They were also more likely to seek mental health support (22%E versus 11%).
- Individuals with mental health-related disabilities were less likely to report their victimization to the police (22% versus 31%). Among those who did, levels of satisfaction with police action were similar to those reported by victims with no such condition.
- Aside from experiences related to victimization, people with mental health disabilities were also overrepresented when it came to various other reasons for police contact. These included calls related to their mental health or substance use or because they had witnessed a crime, but excluded being arrested.
- Persons with mental health-related disabilities more often reported other experiences related to victimization risk, including substance abuse and a history of child abuse and homelessness. This suggests a complex, multidirectional relationship of risk factors and consequences which create a particular intersection of vulnerability.
- Half (51%) of people with a mental health-related disability reported having experienced physical or sexual abuse as a child, and almost a quarter (23%) reported having experienced homelessness. Binge drinking (44%) and drug use (15%) were significantly more common among those with mental health-related disabilities.
- In addition to increased risk of violent victimization, people with mental health-related disabilities also experienced situations associated with social and economic marginalization. Those with mental health disability reported social isolation, inability to work due to illness, lower educational attainment and lower income more often than those without these conditions.
Mental health has been identified as a priority in virtually all spheres of Canadian public life, including the justice, public health, and education systems, as well as both public and private employment sectors (Canadian Mental Health Association n.d.; Mental Health Commission of Canada 2012). As public conversations on this issue continue, ongoing monitoring of the prevalence and outcomes of mental illness is critical to the development of effective policy and program response.
According to the Canadian Survey on Disability (2012), over 1 million Canadians aged 15 years and older—about 4% of the Canadian adult population—live with a mental health‑related disability, with women reporting a higher prevalence than men (Arim 2015; Statistics Canada 2018). Both the Canadian Survey on Disability and the 2014 General Social Survey (GSS) on Canadians' Safety (Victimization) define mental health‑related disability as an emotional, psychological or mental health condition, such as anxiety, depression, bipolar disorder, anorexia, substance abuse and others, which limits daily activities (see Text box 1).
The relationship between victimization and mental illness is complex. While the longitudinal studies required to fully investigate the issue are rare, research has suggested that individuals with some forms of mental illness may be more susceptible to some types of victimization (Devries et al. 2013; Mason and Du Mont 2015; Trevillion et al. 2012). Other research points out that the trauma of victimization can be the catalyst for mental health issues or can exacerbate existing conditions (Kilpatrick et al. 1985), especially for those who experience multiple incidents of violence (Kilpatrick and Acierno 2003). This bidirectionality characterizes the relationship between mental health disability and violent victimization. While cross‑sectional data such as those collected through the 2014 GSS cannot show which of these came first in peoples' experiences, findings presented here serve to underscore the complex relationship between mental health and victimization.
In this Juristat article, information collected through the 2014 GSS from Canadians reporting a mental health disabilityNote is used to contextualize their experiences with the justice system, with a focus on violent victimization, interactions with police and use of victims' support services. Additionally, this article looks at the intersectionality of vulnerability, where mental health disability, substance use, homelessness and a history of child abuse intersect to define an especially vulnerable population. The association between disabilities related to mental health and key markers of societal participation is also reviewed.
Start of text box
Text box 1
How the General Social Survey measures mental health-related disability
The 2014 General Social Survey (GSS) on Canadians' Safety (Victimization) defines a mental health‑related disability as an emotional, psychological or mental health condition, such as anxiety, depression, bipolar disorder, anorexia, substance abuse and others, which sometimes, often or always limits an individual's daily activities. This definition differs slightly from that used by the Canadian Survey on Disability (CSD), which also includes conditions that rarely limit daily activities provided that they prevent a person from doing certain tasks or create a great deal of difficulty when doing them. Because of these differences, results from the GSS and the CSD should not be compared. While official statistics on the prevalence of disability in Canada are generated from the CSD, GSS data are used in this paper because they make possible an analysis of how disability, victimization and other vulnerabilities intersect.
The questions that measure mental health‑related disability used in the 2014 GSS are based on the social model of disability, which emphasizes physical and social barriers that prevent individuals from full participation in all aspects of daily life (Oliver 2013).
It should be noted that the 2014 GSS is designed to measure the experiences of Canadians in the general population, and as such does not collect information from persons residing in institutions, including hospitals, shelters and correctional facilities. This means that findings presented here may not be representative of all Canadians with mental health disabilities. Additionally, individuals with a disability related to mental health which has lasted less than six months and those who indicated that their conditions were managed through treatment to the degree that they no longer interfere with their daily lives are excluded.
End of text box
One in ten people with a mental health disability experiences violence
Research that highlights the link between mental illness and being a victim of crime is well‑established in health and criminogenic studies (Kilpatrick et al. 1985; Kilpatrick and Acierno 2003; Brewerton et al. 2018). In Canada, results from the 2014 GSS support this link. Perreault (2015) found that people with a disability related to mental health experienced violent victimization—sexual assault, physical assault and robbery—at a rate four times higher than those who did not have such a condition.Note Individuals with mental health disabilities reported 236 incidents of violent victimization for every 1,000 people in the 12 months preceding the survey, compared to 66 per 1,000 people with no such condition (Perreault 2015).
Said another way, one in ten (10%) people living with a mental health‑related disability reported having been the victim of violence in the preceding 12 months, while this was the case for 1 in 33 people with no such condition.Note While women with a disability related to mental health were more likely to report violent victimization than their male counterparts (11% versus 8%), there was no statistically significant difference between women and men without such conditions (Chart 1).
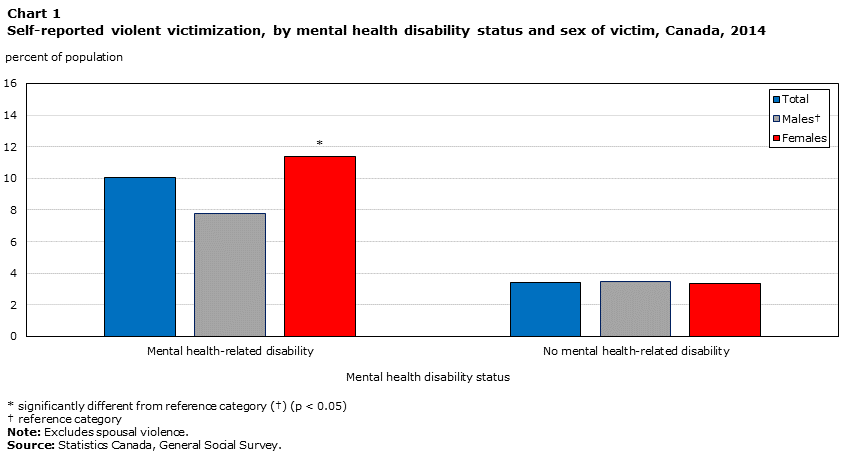
Data table for Chart 1
| Mental health disability status | Total | MalesData table Note † | Females |
|---|---|---|---|
| percent of population | |||
| Mental health-related disability | 10.07 | 7.78 | 11.36Note * |
| No mental health-related disability | 3.42 | 3.50 | 3.35 |
Source: Statistics Canada, General Social Survey. |
|||
Sexual assault was particularly prevalent among women who indicated that they had a mental health‑related disability. Among these women, 7% reported that in the past 12 months, they had experienced a sexual assault. This compares to 2% of women with no mental health disability (Table 1).
In addition to having a higher overall prevalence of violent victimization, those with a mental health‑related disability more often experienced repeat victimization. Close to one third (30%) of victims with a mental health disability reported more than one incident of violence in the previous 12 months, compared to 17% of victims with no such condition.Note This difference reflected the experiences of female victims: among males, no significant difference was detected (Table 1). Some research has suggested that the experience of repeat victimization can have particularly damaging consequences for victims, and also that it may be indicative of a heightened risk profile among individuals (Polvi 1990).
More people with mental health disability victimized by someone they know
Many people with mental health experienced repeated incidents of violence within the context of spousal relationships. Spousal violence—that is, physical and sexual violence that occurs in the context of current and former marriages and common‑law unions—can bring long‑term and life‑altering consequences for victims (Burczycka 2016). As with violent crime overall, people with mental health‑related disabilities were over‑represented as victims of spousal violence: one in eight men and women with a disability related to mental health experienced spousal violence in the five years preceding the survey (12% respectively)—four times more than people with no such condition (3%). In addition, victims of spousal violence who reported a disability related to mental health were considerably more likely to have experienced more than one incident of spousal violence (62%) than their counterparts with no mental health disability (36%).Note Experiences of emotional abuseNote and financial abuseNote in a spousal relationship were also more common among individuals with a mental health‑related disability (Table 2).
In addition to spouses and partners, victims of violence with mental health‑related disabilities were more often victimized by someone else they knew. In half (50%) of the incidents they reported, the offender had been a friend or acquaintance;Note in one in ten (11%) incidents, a family member was involved. This was in marked contrast to victims with no mental‑health related disability, who most often experienced violence from strangers (51% of incidents) (Chart 2). These findings may be correlated with repeated incidents of violence, which are experienced more often by those with mental health disabilities: research has shown that violence that occurs within relationships is more likely to be repetitive (Davis et al. 2006).
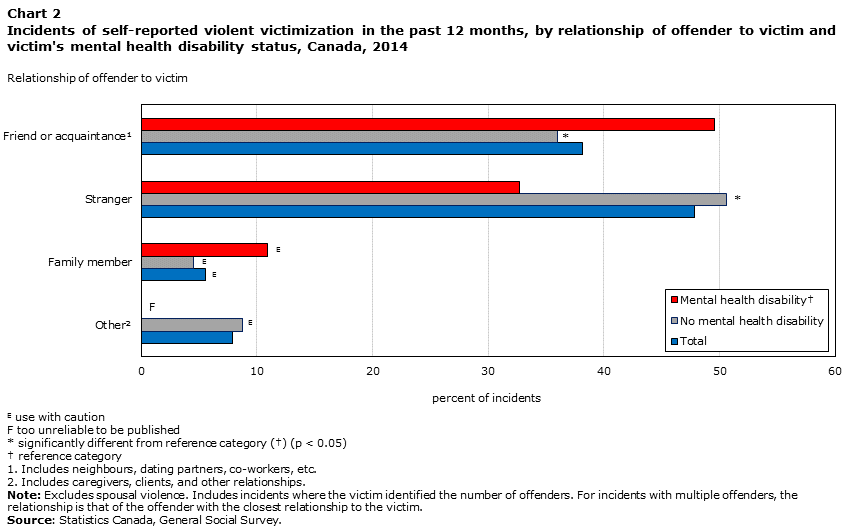
Data table for Chart 2
| Relationship of offender to victim | Total | No mental health disability | Mental health disabilityData table Note † |
|---|---|---|---|
| percent of incidents | |||
| Friend or acquaintanceData table Note 1 | 38.14 | 35.99Note * | 49.53 |
| Stranger | 47.85 | 50.61Note * | 32.71 |
| Family member | 5.55Note E: Use with caution | 4.53Note E: Use with caution | 10.91Note E: Use with caution |
| OtherData table Note 2 | 7.86 | 8.73Note E: Use with caution | Note F: too unreliable to be published |
|
E use with caution F too unreliable to be published
Source: Statistics Canada, General Social Survey. |
|||
Victims with mental health disability report PTSD-like symptoms
The relationship between mental illness and violent victimization is bidirectional, and analyses based on cross‑sectional data such as those collected by the 2014 GSS cannot determine if the presence of mental health‑related disability increases the risk of becoming a victim of crime, or if being a victim of crime results in the onset of a mental health‑related disability. However, the 2014 survey included questions specifically designed to assess whether victimization resulted in symptoms that met the criteria for possible Post‑Traumatic Stress Disorder (PTSD). These questions asked if victims had experienced any of the following symptoms as a result of the victimization: nightmares or intrusive thoughts; having to avoid thinking about the incident and/or avoiding situations that reminded them of it; feeling constantly on guard, watchful or easily startled; or feeling numb or detached from others, activities, or surroundings.Note
Among all victims of violent victimization,Note 14% reported having three or more PTSD‑related symptoms as a result of their experiences (Chart 3). This proportion was substantially higher among those victims who also reported having a mental health disability (29%) than those with no such condition (11%). Despite these findings, the exact relationship between mental health‑related disability and PTSD remains unclear: while these findings may show that victimization can result in PTSD‑like symptoms which may manifest as mental health disability, it is also possible that people with mental health disability may be more susceptible to developing PTSD‑like symptoms.

Data table for Chart 3
| Mental health disability status | Total | No mental health-related disability | Mental health-related disabilityData table Note † |
|---|---|---|---|
| percent | |||
| Victims with 3 or more symptoms | 13.76 | 10.99Note * | 28.64 |
Source: Statistics Canada, General Social Survey. |
|||
More victims with a mental health disability use support services
Victims of violence may access different types of support and assistance in the aftermath of their victimization, including formal services such as counselling, support groups, and programs tailored specifically to victims of crime. Overall, 13% of victims of violence reported that they had made use of this kind of formal assistance (Table 3).Note Uptake was double among victims who indicated that they had a mental health‑related disability compared to those who did not (22%E versus 11%); this may reflect a greater familiarity with accessing services among these individuals, who may have previously sought support for their mental illness.
For example, the 2015 Canadian Community Health Survey found that 60% of women and 50% of men with a diagnosed mood disorderNote had spoken to a professional in the previous 12 months (Statistics Canada 2017). GSS data show a similar pattern, as victims of violence who had a mental health‑related disability were more likely to have spoken with a psychologist, counsellor or social worker about having been victimized, compared to those with no condition (18%E versus 8%). In contrast, both groups were as likely to have made use of a crisis line, a victim service or witness protection program or a sexual assault centre.
Victims with mental health disabilities less likely to report to police
Self‑reported victimization data show that violent crime often goes unreported to the police. Among all victims, police had remained unaware of well over two‑thirds (69%) of incidents of violent crimeNote in the year preceding the 2014 GSS. Individuals with a mental health‑related disability who had been victimized were even less likely to report that police had become involved: 22%E of the incidents that they experienced had been reported to police, compared to 31% among victims without such a condition (Table 3).
It is unclear why individuals with mental health disabilities were less likely to report their victimization experiences to police. For instance, the main reasons they provided for not reporting to police—because they considered the crime to be too minor and not worth the time to report (25%E) or a private matter to be handled informally (18%E)Note —were the same as those most often provided by victims with no mental conditions. Likewise, in instances where police had been made aware of the incident, 66% of all victims reported being somewhat or very satisfied with how police handled the matter—a proportion that was statistically similar between victims with and without a mental health disability (Table 3).
However, the overall perceptions of police held by individuals with mental health disabilities—regardless of whether or not they had been victims of crime—were generally less favorable than those held by people with no such condition. For example, people with disabilities related to mental health were less likely to say that police in their area were doing a good job at enforcing the laws, at being approachable and easy to talk to, at ensuring the safety of citizens, and of treating people fairly. They were also twice as likely to say that overall, they had not very much or no confidence at all in the police (Table 4).
Experiences of victimization had an impact on how individuals with mental health disabilities viewed the police: those who had been victimized rated their perceptions and confidence in police significantly lower than those who had not. However, even among non‑victims, those with disabilities related to mental health had lower perceptions and confidence in police than non‑victims without such conditions; this suggests that individuals' perceptions were influenced by more than their experiences of victimization.Note
Canadians with mental health disabilities overrepresented in contacts with police
The Canadian policing community has recently identified an increase in the number of calls that are not associated with criminal activity, but are instead related to individuals' mental health and substance use. These calls represent a substantial and ever‑increasing component of police work (Standing Committee on Public Safety and National Security 2014). According to the 2014 GSS, over 256,000 Canadians reported that in the previous year, they had come into contact with the police because of problems with their emotions, mental health or alcohol or drug use. This represented 3% of the situations in which Canadians reported having police contact,Note and is likely an underestimate since some populations with higher prevalence of mental illness and substance use are excluded from the GSS (for example, individuals living in drug and alcohol treatment centres, hospitals and shelters).
Not all persons who reported having come into contact with police because of an issue related to emotional or mental health or substance use reported having a long‑term mental illness—in fact, three‑quarters (75%) of those who had contact with police for these reasons did not report having a disability related to mental health.Note This may suggest that for many, the emotional, mental or substance use issues that led to police contact were more acute in nature than the kinds of longer‑term conditions associated with mental health‑related disability. For example, a single instance of public intoxication or aggressive confrontation may result in contact with police, but may not be part of a chronic substance use issue or mental illness.
Nonetheless, people who reported having a mental health disability were over‑represented among Canadians who had come into contact with police due to problems with their emotions, mental health or substance use in the preceding 12 months: 3%E of those who reported having this kind of disability had come into contact with police for these reasons, compared to 1% of those with no such condition (Chart 4).
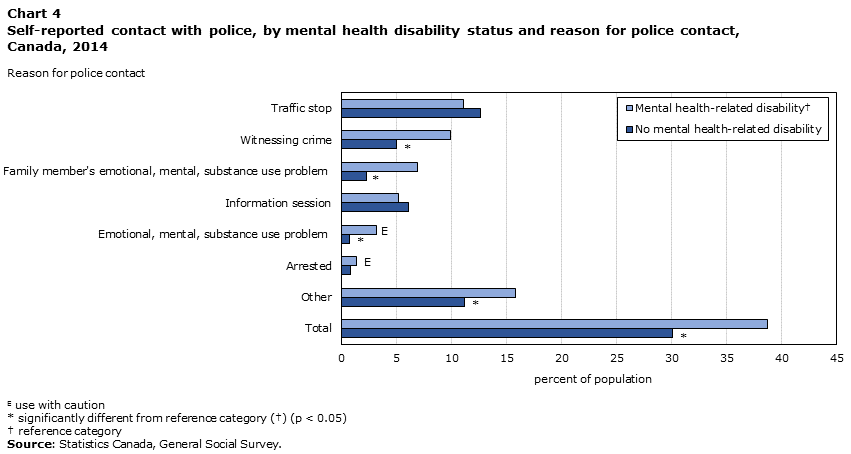
Data table for Chart 4
| Reason for police contact | No mental health-related disability | Mental health-related disabilityData table Note † |
|---|---|---|
| percent of population | ||
| Traffic stop | 12.62 | 11.06 |
| Witnessing crime | 4.98Note * | 9.88 |
| Family member's emotional, mental, substance use problem |
2.32Note * | 6.87 |
| Information session | 6.12 | 5.21 |
| Emotional, mental, substance use problem |
0.70Note * | 3.18Note E: Use with caution |
| Arrested | 0.82 | 1.36Note E: Use with caution |
| Other | 11.18Note * | 15.85 |
| Total | 30.10Note * | 38.70 |
E use with caution
|
||
Aside from contact with police because of issues with their mental health or substance use, those with mental health‑related disabilities were over‑represented when it came to other kinds of contact with police as well. For example, they were more than three times as likely to have had police contact because of an issue with the mental or emotional health or substance use of a family member (7%, compared to 2% of those with no disability related to mental health). Similarly, people who reported having a mental health disability were twice as likely to have been in contact with the police because they had witnessed a crime (10% versus 5% of those with no such condition). As noted in the victims' services community, people who witness crimes and people who live with the daily stress of supporting a family member with mental illness or substance use issues often experience serious mental and emotional consequences themselves (Clark et al. 2008; Pearson 2015).
When it came to having been arrested in the previous year, no difference was found between those with a self‑reported mental health disability and those without (1%E and 1%, respectively). However, since the 2014 GSS did not collect information from people residing in institutions such as prisons, the experiences of those who had been arrested in the previous year and resided in prison during the data collection period were excluded. As a result, these data may underrepresent the criminalization of individuals with mental health‑related disabilities: for instance, federal corrections services data suggest that an estimated 70% of males being admitted into federal custody and 79% of in‑custody adult female federally‑sentenced offenders met criteria for at least one mental disorder (Correctional Services Canada 2015; Correctional Services Canada 2018). Other Canadian research has suggested that people with mental illness are at increased risk of being arrested during their interactions with police, when compared to people with no mental illness involved in similar interactions (Boyce et al. 2015).
Child abuse, homelessness, substance use, linked to mental health, victimization
While a correlation exists between having a mental health disability and being a victim of violence, victimization risk has also been linked to other personal and social characteristics. For example, multiple studies have shown that women and young people are over‑represented as victims of violence; having a history of child abuse, homelessness or substance use are other life experiences which have been found to be highly correlated with victimization (Perreault 2015; Burczycka 2017; Lee and Schreck 2005; Kilpatrick et al. 1997). Each of these factors has been shown to independently increase the risk of violent victimization (Perreault 2015).
According to the 2014 GSS, individuals with mental health‑related disabilities are more likely to be living with several key risk factors for violent victimization—namely, other forms of disability, substance use, a history of homelessness, and a history of child abuse. Furthermore, they are more likely to have low levels of social support and engagement—an important correlation, as some suggest social support and engagement can act as protective factors against the development or worsening of some forms of mental illness following victimization (Carlson et al. 2002) and life stress in general (Cohen 2004).
Mental health disabilities often reported with other disabilities
Mental health‑related disabilities were often reported by people living with another type of disability, including those related to pain, mobility and cognition. Among people who indicated that they had at least one of the other forms of disability measured by the 2014 GSS,Note almost two‑thirds (63%) indicated that they also had a mental health disability that limited their daily lives (Table 5).
The intersection of disability related to mental health and other disabilities is made all the more important when the dimension of violent victimization is added. Canadians who reported living with disabilities reported rates of violent victimization that were double those among people with no disabilities (123 versus 61 incidents per 1,000 population), and violent victimization rates were higher among those with mental health disabilities relative to those with other kinds of disability (Cotter 2018). Further, the likelihood of violent victimization increased significantly with each additional type of disability that was present, including disabilities related to mental health (Cotter 2018).
Binge drinking associated with mental health-related disabilities
For many people, a complex relationship exists between substance use and mental health. The use of alcohol and drugs may cause changes in a person's brain, some of which manifest as mental illness; in addition, individuals with drug or alcohol dependency can experience symptoms analogous to mental illness during withdrawal (Koob and Le Moal 2008). Other studies suggest that while many people with substance use disorders also experience mental illness, these conditions can arise independently of each‑other (Grant et al. 2004). These associations have been noted in clinical research and by experts in the field of addictions treatment, and have been found in relation to so‑called 'hard' drugs (cocaine, heroin, etc.) as well as to alcohol and cannabis and its by‑products (Koob and Le Moal 2008; Grant et al. 2004).
In 2011, the Canadian Centre on Substance Use and Addiction (CCSA) published guidelines meant to inform Canadians on how much alcohol may be consumed in order to limit its acute and chronic health effects (Butt et al. 2011). These guidelines, endorsed by Health Canada, set the limit at no more than 2 drinks a day for women and 3 for men, up to a weekly maximum of 10 for women and 15 for men and with some days of the week kept alcohol‑free.Note According to the 2014 GSS, some types of unsafe drinking are relatively common among Canadians, and are particularly high among those with a mental health‑related disability. Binge drinking—that is, consuming five or more alcoholic drinks on the same occasion—during the previous month was reported by 38% of Canadians with no mental health disability who drank at all during that time. Among those who reported having a disability related to mental health, the proportion was higher (44%) (Table 5).
In contrast, the prevalence of daily alcohol consumption—which goes against the CCSA's recommendation of keeping some days of the week alcohol‑free—was relatively uncommon (5% of Canadians), according to the 2014 GSS. Unlike binge drinking, daily drinking was less common among those who reported a mental health‑related disability (4%) than among those who did not (5%).
Of note, a relatively large proportion of individuals with mental health‑related disabilities reported a complete abstinence from alcohol (31%), compared with people with no such condition (25%). Though GSS data do not provide details on the reasons behind why individuals choose not to drink, abstinence is recommended as both a treatment for alcohol use disorder and a best practice for those taking some types of medications commonly prescribed for mental illness (Butt et al. 2011).
Drug use twice as common for people with mental health disabilities
When it comes to the intersection of drug use and disabilities related to mental health, GSS data show that the use of cannabis products (other than those prescribed by a doctor) and other drugs was more than twice as common among those with this kind of disability.Note When asked about drug use, 15% of those who reported having a disability related to mental health also reported having used cannabis products and/or other drugs such as cocaine or methamphetamine in the month preceding the survey. This compares to 6% of those who did not report such a disability. These proportions were largely reflective of cannabis use, which is considerably more prevalent in Canadian society than other drugs. When it came to other drugs specifically, 2%E of those with a mental health‑related disability reported having used in the past month, compared to 1% of those with no such condition (Table 5).
Multidirectional relationship between substance abuse, mental health, violent victimization
The problematic use of alcohol and other substances has been linked to increased risk of violent victimization in Canada. Using data from the 2014 GSS, Perreault (2015) found that drug use increased the odds of being a victim of violent crime more than any other factor, when controlling for the presence of a mental health‑related disability and other characteristics associated with violent victimization.Note Among those who reported using any drug at least once in the past month, the odds of experiencing violent victimization were almost double. Similar patterns were observed among those who reported binge drinking, in that they were also subject to higher odds of violent victimization after other factors were taken into account.
The correlations between substance use, disability related to mental health and violent victimization reinforce the observation that a complex multidirectionality of risk and consequence underlies the experiences of vulnerable populations. As noted by Perreault (2015) and others, individuals with a self‑reported mental disability often report other risk factors that have been associated with victimization, such as drug use and homelessness. Most often, studies cannot ascertain whether victimization was a result of vulnerable situations such as homelessness or substance use, or whether the trauma related to those experiences brought on mental health disability.
It is important to note that a substance use disorder that limits daily life would itself be defined as a mental health‑related disability within the GSS. Several Canadian population studies have examined mental illness and substance use disorders as separate phenomena. Using self‑reported data from the 2012 Canadian Community Health Survey on Mental Health, Pearson et al. (2013) examined the lifetime prevalence of select mental disorders as well as substance use disorders. They found that 13% of Canadians aged 15 and older met the criteria for having experienced a mood disorder (e.g., a major depressive episode or bipolar disorder) during their lifetimes, while 9% reported having had symptoms of generalized anxiety disorder. Meanwhile, 22% of Canadians met the criteria for a substance use disorder, including problematic use or dependence on alcohol (18%), cannabis use (7%) and the use of illegal drugs other than cannabis (4%).
Almost one-quarter of those with mental health disability have been homeless
The relationship between homelessness and mental illness has been well documented, with mental illness identified as both a potential pathway to and consequence of homelessness (Canadian Institute for Health Information 2007). Findings from the 2014 GSS support this research and show the interrelatedness of homelessness and mental health‑related disability among many Canadians. In 2014, almost 2.5 million Canadians reported that they had at one time been homeless—that is, they had lived in a shelter, on the street, or in an abandoned building, or that they had had to stay with family, friends or in their car because they had nowhere else to go.Note Among them, 16%Note reported having a disability related to mental health. Almost a quarter (23%) of people with this kind of disability reported a history of homelessness, a proportion almost three times that among those with no such condition (8%) (Table 5).
The GSS measures homelessness in two ways: 'hidden' homelessness—that is, having had to stay with family, friends or in one's car because of having nowhere else to go—as well as with the kind of homelessness characterized by having lived in a shelter, on the street or in an abandoned building. The 2014 GSS found that about 20% of those who had experienced any form of homelessness had experienced the latter type, and it is with respect to the latter type that those with mental health‑related disabilities were particularly over‑represented. Proportionally, six times more people with a disability related to mental health reported having had lived in a shelter, on the street or in an abandoned building than did those with no such condition (6% versus 1%). A history of so‑called 'hidden' homelessness was reported by over one in five (21%) people with a mental health disability—three times more often than by those who did not report having this kind of condition (7%) (Table 5).
As with disabilities related to mental health, a history of homelessness has been found to be associated with a higher risk of violent victimization. According to the 2014 GSS, those who reported having experienced either hidden homelessness or having had to live in a shelter, on the street or in an abandoned building had rates of violent victimization that were considerably higher than those who had not (Perreault 2015). Even when multiple other factors associated with victimization risk were accounted for, the odds of being a victim of violence were 80% greater among those with a history of either, or both, forms of homelessness. These findings suggest that a complex relationship between mental illness, homelessness and victimization is present in the lives of many of those affected.
Half of those with mental health disability had experienced child abuse
Numerous studies have established a connection between childhood abuse and mental illness in adulthood, among other physical and psychological consequences (Norman et al. 2012). Data from the GSS show that in Canada, a history of childhood physical or sexual abuseNote was very common among those with self‑reported mental health‑related disabilities. Fully half (51%) of those with this kind of disability reported having been abused during childhood, compared to 29% of those who did not report such a condition (Table 5). Said another way, a history of child abuse was present in one in ten people with a disability related to mental health, compared to one in 25 people with no such condition.Note
A history of child abuse has been shown to have a strong association with violent victimization later in life. Rates of violence in adulthood were considerably higher among those who had been physically and/or sexually abused as children, and having a history of child abuse remained a strong risk factor for violent victimization even after other factors were considered (Perreault 2015). When the relationships between mental health disability and both child abuse and violence in adulthood are considered, a complex picture of intersecting vulnerabilities emerges. Further, factors associated with mental health‑related disability are correlated in other ways; for example, a history of child abuse has been linked to both drug use and having experienced homelessness (Burczycka 2017).
These findings suggest that child abuse, homelessness, substance use and mental health disability represent a particularly important intersection of vulnerabilities when it comes to risk of violent victimization. Theoretical perspectives on vulnerability and victimization have posited that these key factors work together to re‑enforce and re‑create themselves over an individual's life course, amplifying the risk of becoming a victim of violence (Whitbeck et al. 1999).
Social isolation associated with mental health-related disability
Although it is very different from violent victimization, social isolation has been associated with many overlapping consequences for individuals' well‑being, including negative economic, psychological and physical health effects (Locher et al. 2005; Cornell and Waite 2009). Social isolation is also a factor associated with mental health challenges, in a way that is no doubt bidirectional: having a disability related to mental health such as social anxiety, for example, may cause a person to isolate themselves, just as prolonged isolation from meaningful relationships may bring on negative mental health (Kawachi and Berkman 2001). Those who work with vulnerable groups often look for social isolation as an indication that serious mental health problems may exist in a person's life (Locher et al. 2005).
The 2014 GSS provides two measures which illustrate the relationship between social isolation and mental health disability. The first asks Canadians about how many people they have in their lives that they feel close to—that is, who they feel at ease with, can talk to about what is on their mind, or call on for help—excluding people they live with. Over twice as many people who indicated that they had no one in their lives who met this description reported a mental health disability (5%), compared with people who had at least one person in their life that they felt close to (2%) (Table 5).
The 2014 GSS also asks Canadians about their marital status. Having a long‑term partner, such as a legally married or common‑law spouse, can be a protective factor against some of the negative effects associated with social isolation (Umberson and Montez 2010). According to GSS data, those who were married had the lowest prevalence of disability related to mental health (4%), followed by those who were in common‑law unions (5%). The highest prevalence of mental health disability was reported by those who were separated (12%), while those who were divorced or single (never married) also reported a relatively high prevalence (9%, respectively) (Table 6).
Mental health disability associated with lower work participation, income
As with social isolation, an individual's employment status, income and educational attainment can be related to their mental, physical and social well‑being. These factors are reflective of full and active participation in society and appear related to the presence of a mental health‑related disability. GSS data show that individuals with certain sociodemographic profiles have a higher prevalence of disabilities related to mental health.
For example, when it came to people's main activities—whether they were working, studying, ill, retired or taking care of children or their home—about four in ten people whose main activity during the past 12 months was dealing with a long term illness reported a mental health disability (39%) (Table 6).Note In comparison, 14% of those who indicated that their main activity had been looking for work indicated that they had a disability related to mental health, as did 10% of those who had been on parental leave or whose main role was taking care of the home. Mental health‑related disabilities were least common among those who were retired or whose main activity had been working at a paid job or business (4% respectively).
GSS data also show a relationship between mental health‑related disability and income.Note When looking exclusively at those individuals who reported work at a paid job or business as their main activity during the 12 months preceding the survey, those in the lowest two annual household income groups had incidence of mental health‑related disability that were significantly higher than people in the higher groups (Table 6).
It is important to note that GSS data do not show that a mental health‑related disability was the reason for a person's lower income or that a lower income was a reason for a mental health disability. Research has shown that the relationship between income and mental health is bidirectional: while long‑term mental illness can effect employability and earnings, precarious employment and poverty can bring on stress and depression that may become chronic and severe for many individuals (Canadian Institute for Health Information 2007).
In a similar way, the relationship between educational attainment and mental health is bidirectional. Children and youth who struggle with mental health often have trouble with school and may choose not to pursue higher education (Fergusson et al. 2002). Meanwhile, a lower level of education may impact career paths and associated levels of job stability and income—all of which can influence mental health. GSS data show that the prevalence of mental health‑related disability decreased as level of education increased: among people aged 25 and older,Note those whose highest level of education was a high school diploma or less had the highest prevalence of self‑reported mental health disability (7%). Meanwhile, the lowest prevalence of disabilities related to mental health was reported by those who had attained the highest levels of education (university degree above the bachelor's level) (3%) (Table 6).
Summary
As awareness of the causes and outcomes of mental illness continues to grow in Canada, certain patterns emerge. Having a disability related to mental health is associated with a greater risk of violent victimization, and is related to other situations of vulnerability such as homelessness and problem use of drugs and alcohol. While these aspects of individuals' lives are entangled in a multidirectional web of cause and effect, the intersection of these vulnerabilities can provide a roadmap for those looking to intervene with programming and policy. As with other kinds of negative life outcomes, abuse suffered in childhood was related to the presence of mental health‑related disability later in life.
The socioeconomic conditions in which people find themselves may serve as a reflection of their opportunities and capabilities, both of which may be limited by negative mental health. Conversely, the combined pressures of limited opportunity, resource stress and dysfunctional or nonexistent social relationships no doubt brings on or exacerbates mental illness for many. An understanding of these complexities benefits mental health workers, policy makers and concerned community members when it comes to being alert to the needs of individuals who may need help.
Detailed data tables
Survey description
General Social Survey on Canadians' Safety (Victimization)
In 2014, Statistics Canada conducted the victimization cycle of the General Social Survey (GSS) for the sixth time. Previous cycles were conducted in 1988, 1993, 1999, 2004 and 2009. The purpose of the survey is to provide data on Canadians' personal experiences with eight offences, examine the risk factors associated with victimization, examine rates of reporting to the police, assess the nature and extent of spousal violence, measure fear of crime, and examine public perceptions of crime and the criminal justice system.
This report is based on Cycle 28 of the GSS on Victimization conducted in 2014. The target population was persons aged 15 and over living in the Canadian provinces and territories, except for people living full‑time in institutions.
Once a household was selected and contacted by phone, an individual 15 years or older was randomly selected to respond to the survey. An oversample of immigrants and youth was added to the 2014 GSS for a more detailed analysis of these groups.
Data limitations
As with any household survey, there are some data limitations. The results are based on a sample and are therefore subject to sampling errors. Somewhat different results might have been obtained if the entire population had been surveyed. This article uses the coefficient of variation (CV) as a measure of the sampling error. Estimates with a high CV (over 33.3%) were not published because they were too unreliable. In these cases, the symbol "F" is used in place of an estimate in the figures and data tables. Estimates with a CV between 16.6 and 33.3 should be used with caution and the symbol "E" is used. Where descriptive statistics and cross‑tabular analyses were used, statistically significant differences were determined using 95% confidence intervals.
References
Arim, Rubab. 2015. A Profile of Persons with Disabilities Among Canadians Aged 15 Years or Older, 2012. Statistics Canada Catalogue no. 89‑654‑X.
Boyce, Jillian, Cristine Rotenberg and Maisie Karam. 2015. "Mental health and contact with police in Canada, 2012." Juristat. Statistics Canada Catalogue no. 85‑002‑X.
Brewerton, Timothy D., Bonnie Dansky Cotton, and Dean G. Kilpatrick. 2018. "Sensation seeking, binge‑type eating disorders, victimization, and PTSD in the National Women's Study." Eating Behaviors. Vol. 30.
Burczycka, Marta. 2016. "Trends in self‑reported spousal violence in Canada, 2014." In Family violence in Canada: A statistical profile, 2014. Juristat. Statistics Canada Catalogue no. 85‑002‑X.
Burczycka, Marta. 2017. "Profile of Canadians who experience child maltreatment." In Family violence in Canada: A statistical profile, 2015. Juristat. Statistics Canada Catalogue no. 85‑002‑X.
Butt, Peter, Doug Beirness, Louis Gliksman, Catherine Paradis and Tim Stockwell. 2011. Alcohol and Health in Canada: A Summary of Evidence and Guidelines for Low Risk Drinking. Canadian Centre on Substance Use and Addiction. ISBN 978‑1-926705‑79‑8.
Canadian Institute for Health Information. 2007. Improving the Health of Canadians: Mental Health and Homelessness. Canadian Institute for Health Information. ISBN 978‑1-55465‑064‑0.
Canadian Mental Health Association. n.d. Public Policy. Accessed August 9, 2018.
Carlson, Bonnie E., Louise‑Anne McNutt, Deborah Y. Choi, and Isabel M. Rose. 2002. "Intimate partner abuse and mental health: The role of social support and other protective factors." Violence Against Women. Vol. 8, no. 6.
Clark, Cheryl, Louise Ryan, Ichiro Kawachi, Marina J. Canner, Lisa Berkman and Rosalind J. Wright. 2008. "Witnessing community violence in residential neighborhoods: A mental health hazard for urban women." Journal of Urban Health. Vol. 85, no. 1.
Cohen, Sheldon. 2004. "Social relationships and health." American Psychologist. Vol. 59, no. 8.
Cornell, Erin York and Linda J. Waite. 2009. "Social disconnectedness, perceived isolation, and health among older adults." Journal of Health and Social Behavior. Vol. 50, no. 1.
Correctional Services Canada. 2015. "National prevalence of mental disorders among incoming federally‑sentenced men." Research at a Glance. No. R‑357.
Correctional Services Canada. 2018. "National prevalence of mental disorders among federally sentenced women offenders: In custody sample." Research at a Glance. No. R‑406.
Cotter, Adam. 2018. "Violent victimization of women with disabilities, 2014." Juristat. Statistics Canada Catalogue no. 85‑002‑X.
Davis, Robert C., Christopher D. Maxwell and Bruce Taylor. 2006. "Preventing repeat incidents of family violence: Analysis of data from three field experiments." Journal of Experimental Criminology. Vol. 2, no. 2.
Devries, Karen M., Joelle Y. Mak, Loraine J. Bacchus, Jennifer C. Child, Gail Falder, Max Petzold, Jill Astbury and Charlotte H. Watts. 2013. "Intimate partner violence and incident depressive symptoms and suicide attempts: A systematic review of longitudinal studies." PLoS Medicine. Vol. 10, no. 5.
Fergusson, David M., and Lianne J. Woodward. 2002. "Mental health, educational, and social role outcomes of adolescents with depression." Archives of General Psychiatry. Vol. 59, no. 3.
Government of Canada. n.d. Mental health and wellness. Accessed on June 15, 2018.
Grant, Bridget F., Frederick S. Stinson, Deborah A. Dawson, S. Patricia Chou, Mary C. Dufour, Wilson Compton, Roger P. Pickering and Kenneth Kaplan. 2004. "Prevalence and co‑occurrence of substance use disorders and independent mood and anxiety disorders: Results from the national epidemiologic survey on alcohol and related conditions." Archives of General Psychiatry. Vol. 61, no. 8.
Kawachi, Ichiro and Lisa F. Berkman. 2001. "Social ties and mental health." Journal of Urban Health. Vol. 78, no. 3.
Kilpatrick, Dean G. and Ron Acierno. 2003. "Mental health needs of crime victims: Epidemiology and outcomes." Journal of Traumatic Stress. Vol. 16, no. 2.
Kilpatrick, Dean G., Connie L. Best, Lois J. Veronen, Angelynne E. Amick, Lorenz A. Villeponteaux and Gary A. Ruff. 1985. "Mental health correlates of criminal victimization: A random community survey." Journal of Consulting and Clinical Psychology. Vol. 53, no. 6.
Kilpatrick, Dean G., Ron Acierno, Heidi S. Resnick, Benjamin E. Saunders and Connie L. Best. 1997. "A two‑year longitudinal analysis of the relationships between violent assault and substance use in women." Journal of Consulting and Clinical Psychology. Vol. 65, no. 5.
Koob, George F. and Michel Le Moal. 2008. "Addiction and the brain antireward system." Annual Review of Psychology. Vol. 59.
Lee, Barrett A. and Christopher J. Schreck. 2005. "Danger on the streets: Marginality and victimization among homeless people." American Behavioral Scientist. Vol. 48, no. 8.
Locher, Julie L., Christine S. Ritchie, David L. Roth, Patricia Sawyer Baker, Eric V. Bodner and Richard M. Allman. 2005. "Social isolation, support, and capital and nutritional risk in an older sample: Ethnic and gender differences." Social Science & Medicine. Vol. 60, no. 4.
Mason, Robin and Janice Du Mont. 2015. "Advancing our knowledge of the complexity and management of intimate partner violence and co‑occurring mental health and substance abuse problems in women." F1000 Prime Reports. Vol. 7, no. 65.
Mental Health Commission of Canada. 2012. Changing Directions, Changing Lives: The Mental Health Strategy for Canada.
Norman, Rosana E., Munkhtsetseg Byambaa, Rumna De, Alexander Butchart, James Scott and Theo Vos. 2012. "The long‑term health consequences of child physical abuse, emotional abuse, and neglect: A systematic review and meta‑analysis." PLoS Medicine. Vol. 9, no. 11.
Oliver, Mike. 2013. "The social model of disability: Thirty years on." Disability & Society. Vol. 28, no. 7.
Pearson, Caryn. 2015. "The impact of mental health problems on family members." Health at a Glance. Statistics Canada Catalogue no. 82‑624‑X.
Pearson, Caryn, Teresa Janz and Jennifer Ali. 2013. "Mental and substance use disorders in Canada." Health at a Glance. Statistics Canada Catalogue no. 82‑624‑X.
Perreault, Samuel. 2015. "Criminal victimization in Canada, 2014." Juristat. Statistics Canada Catalogue no. 85‑002‑X.
Polvi, Natalie. 1990. "Repeat victimization." Journal of Police Science and Administration. Vol. 17.
Prins, Annabel, Paige Ouimette, Rachel Kimerling, Rebecca Cameron, Daniela Hugelshofer, Jennifer Shaw‑Hegwer, Ann Thrailkill, Fred Gusman and Javaid Sheikh. 2003. "The Primary Care PTSD screen (PC‑PTSD): Development and operating characteristics." Primary Care Psychiatry. Vol. 9, no. 1.
Standing Committee on Public Safety and National Security. 2014. Economics of Policing: Report of the Standing Committee on Public Safety and National Security.
Statistics Canada. 2017. "Accessing mental health care in Canada." Infographic. Statistics Canada Catalogue no. 11‑627‑M.
Statistics Canada. 2018. Table 115‑003: Adults with Disabilities, By Type, Age Group and Sex, Canada, Provinces and Territories. CANSIM (database). Accessed May 23, 2018.
Trevillion, Kylee, Siân Oram, Gene Feder, and Louise M. Howard. 2012. "Experiences of domestic violence and mental disorders: A systematic review and meta‑analysis." PloS One. Vol. 7, no. 12.
Umberson, Debra, and Jennifer Karas Montez. 2010. "Social relationships and health: A flashpoint for health policy." Journal of Health and Social Behavior. Vol. 51, no. 1.
Whitbeck, Les B., Dan R. Hoyt, and Kevin A. Yoder. 1999. "A risk‐amplification model of victimization and depressive symptoms among runaway and homeless adolescents." American Journal of Community Psychology. Vol. 27, no. 2.
- Date modified:
