Health at a Glance
Archived Content
Information identified as archived is provided for reference, research or recordkeeping purposes. It is not subject to the Government of Canada Web Standards and has not been altered or updated since it was archived. Please "contact us" to request a format other than those available.
Trends in the incidence and mortality of female reproductive system cancers
Statistics Canada Catalogue no. 82-624-X
by Tanya Navaneelan
- Highlights
- Uterine cancer incidence at its highest level since 1992; ovarian and cervical cancer incidence decreasing
- Ovarian cancer risk increases with age; uterine and cervical cancer risk rises and falls over the life span
- Ovarian and cervical cancer mortality rates declining over time; uterine cancer mortality rates on the rise in recent years
- Mortality from ovarian and uterine cancers tends to increase with age; cervical cancer mortality more evenly distributed across age groups
- Summary
- What you need to know about this study
- Notes
- Related material for this article
Start of text box
Highlights
- Uterine cancer was the most commonly diagnosed reproductive system cancer in 2010, with a rate of 30.3 new cases per 100,000 women. Uterine cancer incidence was at its highest rate since 1992.
- The risk of a woman being diagnosed with uterine cancer in her lifetime was 1 in 36.
- Ovarian cancer was the deadliest reproductive system cancer, causing 9.5 deaths per 100,000 women in 2010.
- Cervical cancer was more likely to affect younger women than uterine or ovarian cancer. The median age of diagnosis with cervical cancer was 47 years and 28.7% of all new cases were in women under the age of 40.
- The greatest decreases in death from cervical cancer have been made among older women, resulting in a decrease in the median age of death.
End of text box
There were 82,885 new cases of cancer in Canadian women in 2010. Reproductive system cancers accounted for 12.0% of these new cases. The most common types of female reproductive system cancers were cancers of the uterus, ovary and cervix — 9 out of 10 cases developed in one of these three sites (Table 1).
This article presents incidence (new cases) and mortality (deaths) data on uterine, ovarian and cervical cancers. The main data sources are the Canadian Cancer Registry (CCR) and the Canadian Vital Statistics – Death Database.
| Cancer | New cases | Incidence rate (per 100,000 women) |
Percent of all new cancers in women |
|---|---|---|---|
| All reproductive system | 9,957 | 58.0 | 12.0 |
| Uterus | 5,191 | 30.3 | 6.3 |
| Uterus, specified | 5,044 | 29.4 | 6.1 |
| Uterus, NOS* | 147 | 0.8 | 0.2 |
| Ovary | 2,465 | 14.4 | 6.6 |
| Cervix | 1,390 | 8.1 | 1.7 |
| Vagina | 127 | 0.7 | 0.2 |
| Vulva | 487 | 2.8 | 0.6 |
| Other gynecological cancers | 297 | 17.3 | 0.4 |
|
Note: NOS = not otherwise specified Source: Canadian Cancer Registry, Statistics Canada |
|||
Uterine cancer incidence at its highest level since 1992; ovarian and cervical cancer incidence decreasing
In 2010, uterine cancer was the most commonly diagnosed female reproductive system cancer in Canada, with an incidence rate of 30.3 new cases per 100,000 women (Table 2). Between 1992 and 2005 there was no significant change in the rate of uterine cancer; however between 2005 and 2010 there was an increase of 2.5% per year.Note 1,Note 2 This increase resulted in uterine cancer hitting its highest level since 1992, the earliest year captured in the CCR (Chart 1).
| Type of cancer | Incidence | Mortality | ||||
|---|---|---|---|---|---|---|
| New cases | Rate per 100,000 women | Median age at diagnosis | Deaths | Rate per 100,000 women | Median age at death | |
| Uterus | 5,191 | 30.3 | 62 | 919 | 5.4 | 72 |
| Ovary | 2,465 | 14.4 | 62 | 1,637 | 9.5 | 72 |
| Cervix | 1,390 | 8.1 | 47 | 372 | 2.2 | 59 |
| Source: Canadian Cancer Registry, Statistics Canada; Vital Statistics – Death Database, Statistics Canada. | ||||||
Ovarian cancer was the second most commonly diagnosed reproductive system cancer. The rate of ovarian cancer was 14.4 new cases per 100,000 women (Table 2). Between 1992 and 2010 the rate of ovarian cancer decreased by 0.8% annually (Chart 1).

Cervical cancer was the third most commonly diagnosed reproductive system cancer with a rate of 8.1 new cases per 100,000 women (Table 2). Like ovarian cancer, the incidence of cervical cancer has declined over time, falling by 2.1% annually between 1992 and 2005. However, this decrease has leveled off in recent years and, between 2005 and 2010, there was no significant change in the rate (Chart 1).
Research into the decline in the rate of cervical cancer indicates that this is most likely the result of cervical cancer screening programs.Note 3,Note 4,Note 5 These programs have helped to increase the number of pre-cancerous conditions caught before they develop into invasive cancer.
Start of text box
Cervical cancer screening
Unlike uterine and ovarian cancer, cervical cancer has a widely available screening test: the Papanicolaou (Pap) test. Most cervical cancer occurs in women who have never undergone screening or who have had a long interval between Pap tests.Note 6 In 2012, 90.2% of women aged 21 to 69 reported having had a Pap test in their lifetime, although only 74.2% had one within the past three years, as recommended. In addition, the percentage of women who had a Pap test within the past three years decreased over time, down from 77.5% in 2000.Note 7
End of text box
Ovarian cancer risk increases with age; uterine and cervical cancer risk rises and falls over the life span
A woman’s age can affect her risk of developing each type of reproductive system cancer. Women in their sixties and early seventies had the highest risk of uterine cancer (Chart 2). The peak was in women between the ages of 60 to 64, who had a rate of 99.0 new cases per 100,000 women. Around this peak, incidence rates increased with age for women aged 25 to 59 while they decreased with age for women 65 and older.
Over time, the highest levels of uterine cancer risk have shifted to younger women. In 2010, the medianNote 8 age of diagnosis with uterine cancer was 62 years. In contrast, in 1992, the median age of diagnosis was 66 years and women in their seventies had the highest incidence rate.
Unlike uterine cancer, ovarian cancer rates tended to increase with age. Ovarian cancer was relatively rare in women aged 25 to 29, who had a rate of 2.4 new cases per 100,000. In comparison, incidence was more than 20 times higher in women aged 85 and older who had a rate of 46.1 new cases per 100,000 women (Chart 2). Although risk increased with age, 6.4% of ovarian cancer cases were diagnosed in women under the age of 40 compared with 2.6% of uterine cancer cases. Similar to uterine cancer, the median age of diagnosis with ovarian cancer was 62 years.
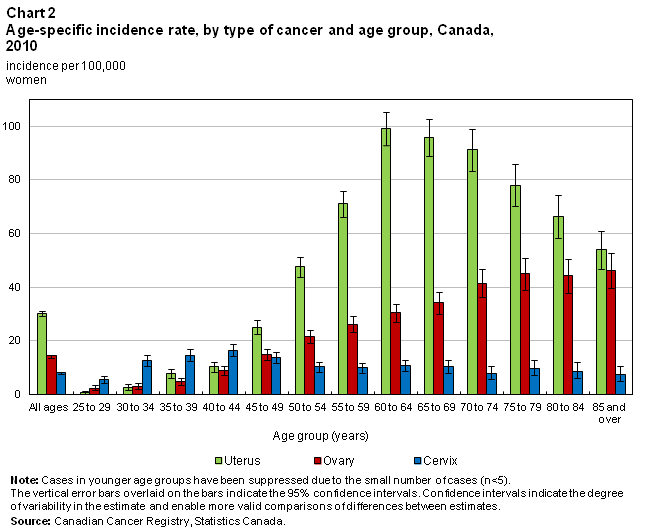
Women in their early forties had the highest risk of cervical cancer. Women aged 40 to 44 had a cervical cancer incidence rate of 16.6 new cases per 100,000 women. Similar to uterine cancer, rates were lower on either side of this peak, although the risk was more evenly distributed across the age groups (Chart 2).
Compared with the other two main reproductive cancers, cervical cancer was more likely to affect younger women with 28.7% of cases occurring in women under the age of 40. Despite cervical cancer having the lowest overall incidence, women aged 25 to 45 had a higher rate of cervical cancer than of uterine or ovarian cancer. Additionally, the median age at which women were diagnosed with cervical cancer was 47 years, considerably lower than for the other two cancers.
Start of text box
Lifetime risk
Lifetime risk estimates the risk of a newborn child developing a particular type of cancer at some point during their lifetime.Note 9,Note 10 The lifetime risk of developing uterine cancer was 1 in 36 (or 2.8%) in 2010.Note 11 Ovarian cancer had a lower lifetime risk of 1 in 71 (or 1.4%), and cervical cancer had the lowest lifetime risk of 1 in 155 (or 0.6%).
End of text box
Ovarian and cervical cancer mortality rates declining over time; uterine cancer mortality rates on the rise in recent years
While incidence figures represent the number of new cases of a disease, mortality data reflect the number of deaths from that disease. Cancer was the leading cause of death for women in 2010,Note 12 and reproductive cancers accounted for 9.2% of these deaths.
Although uterine cancer was the most commonly diagnosed reproductive cancer, ovarian cancer caused the greatest number of deaths. In 2010, the mortality rate from ovarian cancer was 9.5 deaths per 100,000 women (Table 2). Despite the relatively high mortality rate, the risk of death due to ovarian cancer has decreased over time. Between 1974 and 2010, the rate decreased by 0.7% annually (Chart 3).Note 1
Ovarian cancer mortality was higher than mortality from other reproductive cancers largely because most women are not diagnosed with ovarian cancer until it is at an advanced stage and the cancer has already spread beyond the ovaries. This is mainly because ovarian cancer lacks clearly identifiable early symptoms.Note 13,Note 14
The mortality rate for uterine cancer was 5.4 deaths per 100,000 women, making it the second deadliest form of reproductive cancer (Table 2). While uterine cancer mortality saw declines of 1.4% per year between 1974 and 2000, these declines came to an end between 2000 and 2010, when the rate increased by 0.9% annually (Chart 3).

Cervical cancer deaths were the lowest of the three main reproductive cancers with a rate of 2.2 deaths per 100,000 women (Table 2). Not only has mortality from cervical cancer been relatively low but the rate has also been declining over time. Mortality in 2010 was less than a third of what it was in 1974, a decline of 3.2% annually (Chart 3). The decline in deaths from cervical cancer, like the decline in new cases, is likely a result of cervical cancer screening programs.Note 6,Note 7
Mortality from ovarian and uterine cancers tends to increase with age; cervical cancer mortality more evenly distributed across age groups
A woman’s risk of death from reproductive cancer, like her risk of diagnosis, is affected by her age. Death from ovarian cancer increased steadily with age, with women 85 and older having the highest mortality at a rate of 58.7 deaths per 100,000 women (Chart 4). This is similar to the pattern seen with new cases of ovarian cancer, which also tended to increase with age (Chart 2).
Similarly, deaths from uterine cancer also increased with age, peaking in the oldest age group. Women aged 85 and older had a uterine cancer mortality rate of 44.6 deaths per 100,000 women (Chart 4). By comparison, diagnosis with uterine cancer peaked among women in their early sixties.
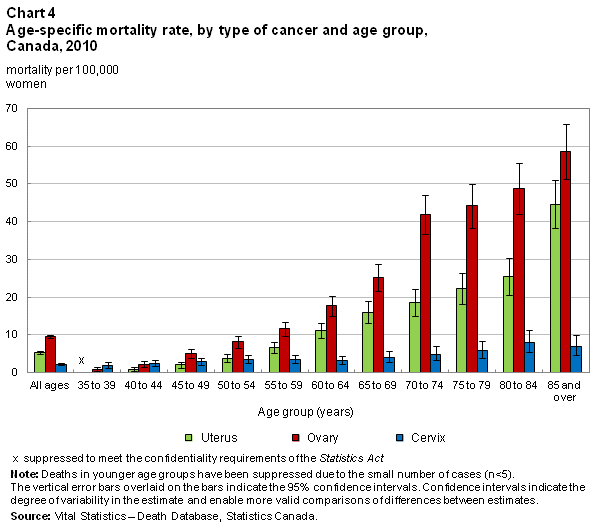
Deaths from cervical cancer were more evenly distributed across the life span than ovarian or uterine cancer deaths, however there was still a general trend of increasing mortality with increasing age (Chart 4). The highest mortality was in women aged 80 to 84 years (7.9 per 100,000 women), followed by women aged 85 and older (6.9 per 100,000 women).Note 15 Like uterine cancer, cervical cancer mortality peaked at a later age than diagnosis, which was highest among women in their early forties.
Even though cervical cancer had a relatively low mortality rate, it presented a greater risk of death for younger women than ovarian or uterine cancer. In women under 45 years of age, the risk of death from cervical cancer was greater than death from either of the other two cancers (Chart 4).
Like the median age at diagnosis, the median age of death was the same for women with uterine and ovarian cancer, and was significantly younger for women with cervical cancer (Table 2). In addition, while the median age of death from uterine and ovarian cancer has risen over time, the median age has decreased for cervical cancer. The median age of death from cervical cancer in 2010 was 59 years, a decrease of one and a half years since 1974. In comparison, over the same period, the median age at death from ovarian cancer increased by nine and a half years and by three and a half years for uterine cancer. The decline in the median age at death from cervical cancer occurred because the greatest declines in mortality have been made in older women. For example, there was a 76.6% decrease in the rate of death from cervical cancer in women aged 70 to 74 compared with a 32.0% decrease in women aged 35 to 39.
Summary
Cancers of the reproductive system accounted for 12.0% of all newly diagnosed cancer cases in Canadian women in 2010. Uterine cancer was the most commonly diagnosed with 30.3 new cases per 100,000 women, its highest rate since 1992. While the risk of death from ovarian cancer was almost twice that of uterine cancer, ovarian cancer mortality has been steadily decreasing since 1974. On the other hand, the rate of death from uterine cancer increased between 2000 and 2010. Cervical cancer had the fewest new cases and deaths, but was also the most likely to affect younger women, with the lowest median age of diagnosis and death.
Start of text box
What you need to know about this study
Classification of key concepts
For incidence data, the cancers discussed in this article were defined using the International Classification of Disease for Oncology, Third Edition (ICD-O-3)Note 16 as follows: Uterus: C54.0 - C54.9, C55.9; Ovary: C56.9; Cervix: C53.0 - C53.9. All cancers exclude the following histologies: 9050-9055, 9140 and 9590-9992. Only malignant cases were included.
Mortality data were classified according to the International Statistical Classification of Diseases and Related Health Problems, Tenth Revision (ICD-10),Note 17 Ninth Revision (ICD-9),Note 18 and Eighth Revision (ICD-8).Note 19 The following definitions were used to determine cause of death:
Cancer of the uterus: ICD-10 - C54, C55; ICD-9 - 182, 179; ICD-8 - 182
Cancer of the ovaries: ICD-10 - C56; ICD-9 - 183; ICD-8 - 183
Cancer of the cervix: ICD-10 - C53; ICD-9 - 180; ICD-8 - 180
Data sources
Cancer incidence data are from the Canadian Cancer Registry (CCR), a dynamic person-oriented, population-based database maintained by Statistics Canada. The CCR contains information on cases diagnosed from 1992 onward, compiled from reports from every provincial/territorial cancer registry.
Analyses were carried out using a tabulation master file. This master file was created by applying the International Rules for Multiple Primary CancersNote 20 to a copy of the CCR (dated January 10, 2014) limited to invasive tumours and in situ bladder tumours.
Mortality data are from the Canadian Vital Statistics – Death Database, also maintained by Statistics Canada. Mortality data are based on information provided by the provincial and territorial vital statistics registrars. Canadians who died while residing outside of Canada were excluded from the analysis because of inconsistencies in the reporting of deaths by non-Canadian jurisdictions.
Supplementary data on screening are from the Canadian Community Health Survey (CCHS).Note 7
Trend analysis
Trends in age-standardized incidence and mortality rates over time were determined using the Joinpoint Regression Program (v.4.0.4) distributed by the SEER (Surveillance Epidemiology and End Results) program.Note 21
All trend analyses were performed using age-standardized rates. Since cancer is more likely to occur in older people, the age structure of a population will have a strong influence on the incidence and mortality rates observed. To allow for more valid comparisons over time, age-standardized rates are used to control for differences in population age-structure. The age-standardized rate is the rate that would occur if the population of interest had the same age-structure as the standard population. The standard population used here is the July 1, 1991 Canadian population.
Limitations
Incidence data may exclude some cases that were reported late or not processed in time for the final file. As the CCR is a dynamic database previous years of data are updated with these missing cases. Therefore, the most recent years of data may slightly underestimate the actual incidence.
Some women in the population may not be at risk for certain reproductive system cancers if the organs where these cancers form have been removed (e.g. hysterectomy). These women were not removed from the at-risk population in this analysis.
New revisions of the ICD are developed periodically to maintain the classification’s currency. The mortality data reported in this article use three revisions of the ICD coding system. Different revisions may classify certain causes of deaths differently, resulting in the classification of deaths being affected by the year in which they occurred. While differences between the revisions used in this article are minimal for cancers of the reproductive system, discrepancies based on the ICD version used are possible.Note 22,Note 23,Note 24
End of text box
Tanya Navaneelan is an analyst with the Health Statistics Division.
The author wishes to acknowledge Gregory Christ, Larry Ellison and Dianne Zakaria for their contributions.
Notes
Additional information
- For more statistics and analysis on the health of Canadians and the health care system, visit the Health in Canada module. This module is accessible from our website, under Features.
Data sources
Bibliographic references
- Date modified:
